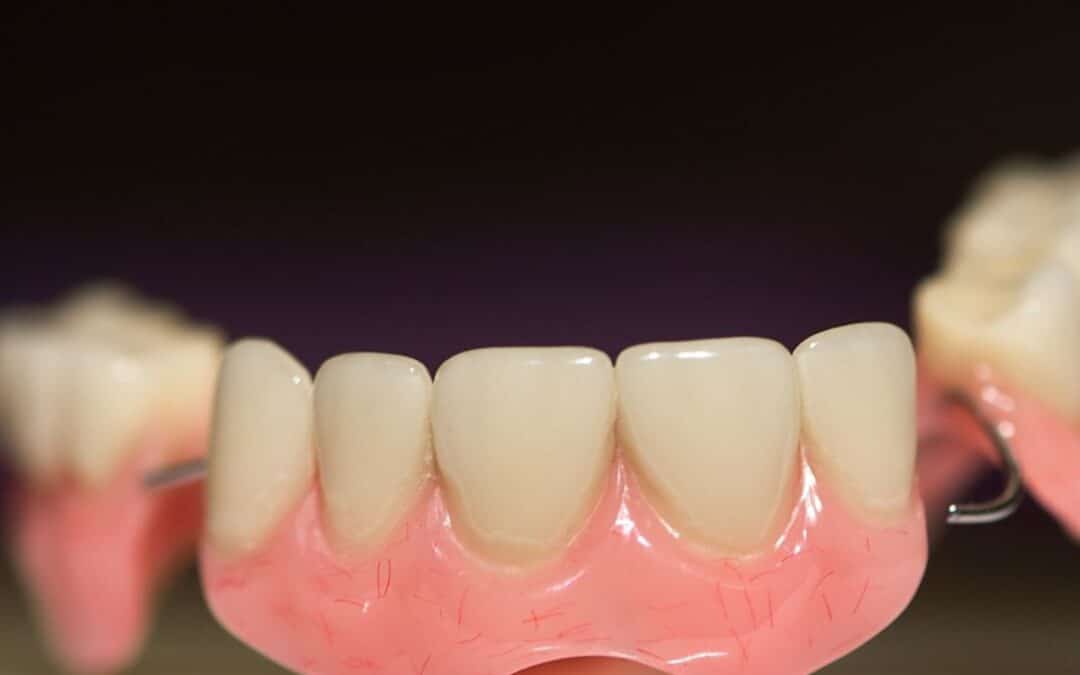
by 110 Dental & Orthodontics | Mar 20, 2026 | Dentures
Sore spots can turn a confident smile into daily discomfort. Many denture wearers notice tender areas on their gums after weeks or even months of use. These spots often stem from friction or pressure. Yet simple changes in routine can keep your mouth comfortable and healthy. This guide shares practical steps to stop irritation before it starts.
Understanding What Causes Sore Spots with Dentures
Dentures press against soft gum tissue every day. Poor fit ranks as the top culprit. Over time, jawbones shrink naturally, so dentures that once felt snug begin to rub. New dentures also trigger adjustment soreness as tissues adapt.
Poor hygiene adds another layer. Food particles and bacteria trapped underneath create inflammation. Loose pieces shift during chewing and create hot spots. Dry mouth or certain habits like smoking worsen the issue by reducing saliva that cushions tissues.
Daily Habits That Protect Your Gums
Start each morning with a quick inspection. Remove dentures and rinse your mouth with warm water. Brush gums gently with a soft toothbrush to stimulate blood flow and clear debris.
Clean dentures every night. Use a denture-safe brush and mild cleanser. Soak them in a denture solution while you sleep. This routine removes plaque and prevents bacteria buildup that leads to soreness.
Take breaks during the day. Remove dentures for short periods if possible. Nighttime removal gives gums full rest and speeds healing.
Eat softer foods at first. Cut items into small pieces and chew slowly on both sides. Avoid sticky or hard snacks that force dentures to slip.
Effective Home Remedies for Fast Relief
Warm saltwater rinses work wonders. Mix half a teaspoon of salt in a glass of warm water. Swish gently four or five times daily. The solution calms inflammation and cleans minor sores.
Apply a cold compress to the outside of your cheek for ten minutes. It reduces swelling without touching the sore area directly.
Keep dentures stable with a thin layer of adhesive when needed. It limits movement and cuts friction on tender spots.
Stay hydrated throughout the day. Water keeps the mouth tissues moist and less prone to irritation.
Professional Care Keeps Problems Away
Regular checkups catch fitness issues early. Dentists can spot small changes in gum shape and make precise adjustments. A quick reline often restores comfort without major changes.
Patients in Whitehouse, TX, who rely on dentures know how small tweaks prevent recurring pain. Consistent visits ensure prosthetics match evolving mouth contours.
| Common Cause |
Prevention Tip |
| Ill-fitting dentures |
Schedule adjustments every 6-12 months |
| Bacteria buildup |
Clean daily and soak overnight |
| New denture adjustment |
Wear gradually and use adhesive |
| Jawbone changes over time |
Get professional relines as needed |
Trending FAQs About Denture Sore Spots
What causes sore spots from dentures? Friction from poor fit or shifting prosthetics irritates gums. Bacteria trapped underneath can worsen the problem.
How long do denture sores usually last? Minor spots heal in a few days with proper care and removal at night. Persistent ones need professional attention.
How can I soothe sore spots at home? Warm saltwater rinses, cold compresses, and short breaks from wearing dentures bring quick relief.
Should I keep wearing dentures if they hurt? Remove them temporarily and rinse your mouth. See a dentist if pain lasts more than a few days.
Can poor hygiene lead to infections? Yes. Clean dentures and gums daily to stop bacteria from causing ulcers or denture stomatitis.
When do I need a denture reline? If soreness returns often or dentures feel loose, a reline restores the snug fit your gums need.
Long-Term Strategies for Lasting Comfort
Track any changes in your bite or speech. These clues signal that dentures need attention. Replace worn brushes and cleansers on schedule to maintain top hygiene.
Consider your overall health, too. Conditions like diabetes can slow healing, so coordinate with your doctor. Consistent routines build habits that protect gums for years.
If you are searching for a dentist near Whitehouse, TX, experts agree that proactive care stops small irritations from becoming big problems.
Preventing sore spots from dentures comes down to fit, cleanliness, and daily attention. Follow these steps and enjoy meals, conversations, and smiles without hesitation. Your mouth will thank you every day. Schedule an appointment to keep your dentures feeling just right.

by 110 Dental & Orthodontics | Mar 13, 2026 | Invisalign
Finishing your Invisalign journey brings real excitement. You finally enjoy the straight, confident smile you worked so hard to create. Yet many people notice small changes months or years later. Teeth begin to drift slightly. This common experience stems from natural biological processes rather than any failure on your part.
Understanding the Biology Behind Tooth Movement
Teeth are not locked permanently in place. Each tooth sits in a socket held by flexible periodontal ligaments. During Invisalign treatment, these fibers stretch and reorganize. When aligners are removed, the ligaments still hold memory of the original positions. They continue to exert gentle pulling forces.
At the same time, the bone surrounding the roots needs time to fully remodel and harden in the new locations. This stabilization process can take 12 to 24 months or longer. During this period, even minor daily pressures can cause teeth to shift gradually.
Why Teeth Shifting After Invisalign Happens
Teeth shifting after invisalign is a natural response of the mouth returning toward its previous state. The ligaments and bone are still adapting. Without complete stabilization, everyday forces easily influence tooth positions.
Your tongue pushes against teeth thousands of times each day. Lips and cheeks apply constant light pressure. Chewing, speaking, and swallowing create subtle movements. When the bite is perfectly balanced, these forces remain even. Any imbalance concentrates stress on certain teeth and encourages drift over time.
Daily Habits That Accelerate Shifting
Certain habits increase the likelihood of movement after treatment. Nighttime teeth grinding or clenching delivers strong, repeated forces. Nail biting, using teeth to open packages, or tongue thrusting adds extra pressure. Even poor posture that changes head position can slowly affect jaw alignment.
These repeated actions compound. What starts as tiny shifts can become more noticeable over months if left unchecked.
The Role of Age and Genetics
Age plays an important part, too. As adults get older, jawbones slowly change in shape and density. Teeth naturally tend to drift forward a small amount each decade. Some people inherit a stronger genetic predisposition to movement due to bone structure or soft-tissue patterns.
If your original crowding or spacing was significant, the risk of later shifting rises. Teeth that require major rotation or expansion often need more time to settle securely.
Key Factors Contributing to Post-Invisalign Movement
| Factor |
How It Affects Teeth |
Typical Timeframe |
| Ligament Memory |
Fibers pull toward their original positions |
First 12–18 months |
| Bone Remodeling |
New bone hardens slowly around roots |
Up to 24 months |
| Daily Oral Pressures |
Tongue, lips, and cheeks push constantly |
Ongoing |
| Bruxism & Clenching |
Heavy nighttime forces on teeth |
Every night |
| Aging Jaw Changes |
Bone density and shape evolve |
Over many years |
Research indicates that some degree of orthodontic relapse occurs in a notable percentage of clear aligner cases during the early post-treatment phase. These numbers show how common minor movement can be.
Patients who receive our invisalign treatment in Whitehouse, TX, benefit from clear explanations about these processes. Understanding the “why” helps them recognize early signs and take simple protective steps.
Trending FAQs About Teeth Shifting After Invisalign
- How soon after Invisalign can teeth start shifting? Subtle changes can begin within a few weeks. Most noticeable movement usually appears within the first year as tissues adapt.
- Is some movement after Invisalign normal? Light settling is common while ligaments and bone stabilize. Larger shifts usually signal stronger ongoing forces.
- Do habits like grinding really cause teeth to move? Yes. Repeated heavy pressure from grinding or clenching can push corrected teeth out of alignment over time.
- Does age influence how much teeth shift? It does. Older jaws undergo gradual changes that can increase natural forward drifting.
- Can an imperfect bite speed up shifting? Definitely. An uneven bite creates focused pressure points that accelerate unwanted tooth movement.
Protecting Your Results Long Term
Your new smile deserves to stay beautiful for years to come. The reasons teeth shift after Invisalign come down to biology, daily forces, and personal habits. Staying aware of small changes and maintaining regular check-ins with your orthodontic provider in Whitehouse, TX, makes all the difference.
By understanding these natural processes, you gain the knowledge needed to protect your investment in a straighter smile. Small, consistent attention keeps your results looking their best.
Contact us today to review your smile and ensure it stays perfectly aligned for years ahead.

by 110 Dental & Orthodontics | Mar 6, 2026 | Dental Care
Dental implants can restore your smile and confidence for many years. Still, many people worry whether simple daily habits might quietly put their investment at risk. The short answer is yes. Neglecting consistent oral care allows bacteria to gather around the implant. This can quickly lead to inflammation and more serious complications. Knowing how this happens empowers you to protect your new teeth effectively.
How Dental Implants Work and Why They Need Extra Care
Dental implants function as artificial roots placed directly into the jawbone. A realistic crown sits on top, giving you a natural look and feel. However, unlike natural teeth, implants do not have the same protective structures. The soft gum tissue around them is more vulnerable to bacterial attack. Plaque can build up rapidly at the gum line if cleaning is inconsistent.
The Direct Link Between Poor Hygiene and Infection
When brushing and flossing become irregular, harmful bacteria form a sticky biofilm. This biofilm hardens into tartar that regular brushing cannot remove. The result is inflammation of the gums around the implant, known as peri-implant mucositis. If left unaddressed, this condition advances deeper. It begins to affect the bone supporting the implant. At this stage, it develops into a dental implant infection that can threaten the stability of the entire restoration.
Early warning signs often appear subtly. You may notice red or swollen gums near the implant. Persistent bad breath or a metallic taste can also signal trouble. In some cases, pus or slight loosening of the crown occurs. Pain is not always the first symptom, which is why regular self-monitoring matters.
Simple Daily Habits That Protect Your Implants
Protecting your dental implants starts with smart daily routines.
- Brush twice a day using a soft-bristled toothbrush. Angle the bristles gently toward the gum line.
- Use floss threaders, interdental brushes, or a water flosser to clean the hard-to-reach areas around the implant. An antimicrobial mouthwash adds an extra layer of defense.
- Replace your toothbrush every three months to maintain effectiveness.
The Role of Professional Dental Care
Home care works best when paired with regular dental visits. Our dentists can detect early changes through careful examination and X-rays. They perform specialized cleanings that reach areas you might miss. These checkups help catch small problems long before they become serious.
That is why many patients in the area benefit greatly from our routine dental care in Whitehouse, TX. Consistent professional support combined with strong home habits creates the strongest defense for long-term implant success.
What the Numbers Reveal
Research highlights just how important good hygiene is. Consider these key statistics:
| Condition |
Prevalence |
Main Trigger |
| Peri-implant mucositis |
Up to 88% of patients |
Poor plaque control |
| Peri-implantitis |
9% – 45% |
Untreated bacterial buildup |
| Risk of significant bone loss |
Significantly higher |
Inconsistent daily oral hygiene |
These figures show why even small lapses in routine can lead to bigger issues over time. The good news is that early inflammation is often reversible with improved care.
Trending FAQs About Dental Implant Infection
- What is peri-implantitis? Peri-implantitis is an advanced inflammatory condition that affects both the gum and the bone around a dental implant, similar to severe gum disease.
- Can dental implant infection happen years after placement? Yes. Infections can develop even many years later if oral hygiene slips or other risk factors increase.
- Do infected dental implants always cause pain? Not necessarily. Early stages can be painless, making regular checkups and self-monitoring very important.
- What is the best way to clean around dental implants? Use a soft toothbrush, floss threaders or water flossers daily, and incorporate an antimicrobial rinse for better bacterial control.
- Is poor oral hygiene the only cause of implant problems? It is the most common cause, but factors like smoking, diabetes, or previous gum disease can raise the risk further.
Taking care of your dental implants does not have to be complicated. Small, consistent changes in your daily routine can make a huge difference. Stay alert to early signs, maintain excellent home care, and work closely with our local dentist in Whitehouse, who focus on long-term results. Your healthy, confident smile is worth the effort. Contact us today and give your implants the protection they deserve for years to come.

by 110 Dental & Orthodontics | Feb 27, 2026 | Veneers
Picture this: You’ve finally decided to transform your smile with veneers, envisioning that confident grin lighting up every conversation and meal. But then doubt creeps in—what if these thin porcelain shells throw off your words or how you chomp into your favorite foods? It’s a valid worry. Many folks hesitate right at this crossroads, fearing the unknown. The good news? With modern techniques, these concerns are often short-lived blips on the road to a radiant smile. Let’s dive into the facts, ease your mind, and arm you with what you need to step forward boldly.
What Are Dental Veneers, Anyway?
Dental veneers are custom-made facades, usually crafted from durable porcelain or composite resin, that bond to the front of your teeth. They mask chips, gaps, discoloration, or minor misalignments, delivering a natural, polished look. Think of them as tailored armor for your smile—sleek and unobtrusive.
In cosmetic dentistry, veneers shine for their minimally invasive prep. Your dentist lightly etches the enamel for adhesion, preserving most of your natural tooth. This approach sets them apart from bulkier options like crowns, which cover the entire tooth. Results? A brighter, more even smile without drastic reshaping.
How Veneers Can Influence Your Speech
Speech tweaks top the list of pre-treatment jitters. The tongue dances with teeth edges during sounds like “s,” “th,” or “f.” New veneers add a whisper of thickness, potentially nudging your tongue into unfamiliar territory. This might spark a temporary lisp or slight slur, especially in the first days.
Rest easy—it’s rarely permanent. Studies show most patients adapt swiftly as the brain recalibrates. The key? Precise design. Skilled providers mimic your natural contours, minimizing disruption. If changes linger beyond two weeks, a quick polish often fixes it. Remember, this phase passes, leaving you to chat freely again.
The Real Scoop on Veneers and Your Bite
Biting down feels intuitive until something shifts. Veneers aim to enhance, not overhaul, your occlusion—the way teeth meet. Properly fitted ones distribute pressure evenly, potentially easing strain from uneven wear. Yet, initial sensitivity or a “high spot” can make chewing feel off-kilter at first.
Here’s the upside: Veneers often refine bite harmony. For instance, they can level worn edges, promoting smoother jaw function. Complications like persistent misalignment are rare when starting with a thorough exam. Your dentist evaluates your current bite via impressions and digital scans, ensuring seamless integration.
When exploring our veneers treatment in Whitehouse, TX, you’ll find options tailored to preserve that natural chew. Local expertise ensures adjustments align perfectly with your daily habits, from crisp apple bites to hearty steak slices.
Navigating the Adjustment Period After Veneers
Day one post-placement? Your mouth buzzes with novelty. Saliva flow might spike as nerves settle, and textures feel amplified. This honeymoon haze typically fades in 24-48 hours. By week one, speech flows smoother, and bites land true.
Patience pays off. Hydrate well, opt for soft foods like yogurt or smoothies, and practice enunciation with tongue twisters. If discomfort persists, flag it—minor tweaks restore balance fast. Long-term? Over 95% of patients report no ongoing issues, per dental research.
| Common Veneer Concern |
Typical Impact |
Adaptation Timeline |
Success Insight |
| Speech Alteration |
Temporary lisp or slurring |
1-2 weeks |
98% resolve without intervention |
| Bite Discomfort |
Mild sensitivity or uneven feel |
3-7 days |
Improves occlusion in 85% of cases |
| Overall Satisfaction |
High confidence boost |
Immediate post-adjustment |
95.5% 10-year survival rate |
This table draws from clinical data, highlighting how fleeting hurdles lead to lasting wins.
Practical Tips to Ease Into Your New Smile
Preparation sets the tone. Before treatment, discuss speech patterns and bite quirks with your provider. They might suggest phonetic tests to fine-tune shapes.
Post-care matters too. Skip sticky candies that tug at bonds. Brush gently with a soft toothbrush, and floss daily to shield edges. Regular check-ins catch tweaks early. These steps not only safeguard your investment but amplify comfort from the get-go.
If you are searching for a cosmetic dentist near you, prioritize those versed in smile simulations—digital previews let you “try on” results, spotting potential speech or bite snags upfront.
Trending FAQs on Veneers, Speech, and Bite
Curious minds flock to these queries online. Based on popular searches, here’s the lowdown in quick bites:
- Do veneers cause a permanent lisp? No, lisps are transient. Your tongue adapts as muscle memory kicks in, usually within days. Persistent cases? A simple edge adjustment resolves it.
- How long until my bite feels normal after veneers? Most notice full comfort by week’s end. Start with softer eats to bridge the gap smoothly.
- Can veneers fix an existing bite problem? Absolutely, if minor. They even surfaces for better alignment, but severe issues might pair with orthodontics.
- Will veneers make my teeth feel bulkier when talking? Initially, yes—a subtle shift. But custom fits ensure they blend like your originals.
- What if speech changes bother me right away? Contact your dentist pronto. Early refinements prevent worry and speed recovery.
These answers stem from patient forums and expert insights, proving veneers prioritize function alongside flair.
Veneers aren’t just about aesthetics—they’re a gateway to unhindered expression and enjoyment. You’ve got the tools now to tackle fears head-on, knowing any ripples are ripples, not waves. Ready to claim that effortless smile? Schedule an appointment today and let your words—and bites—shine without a second thought.
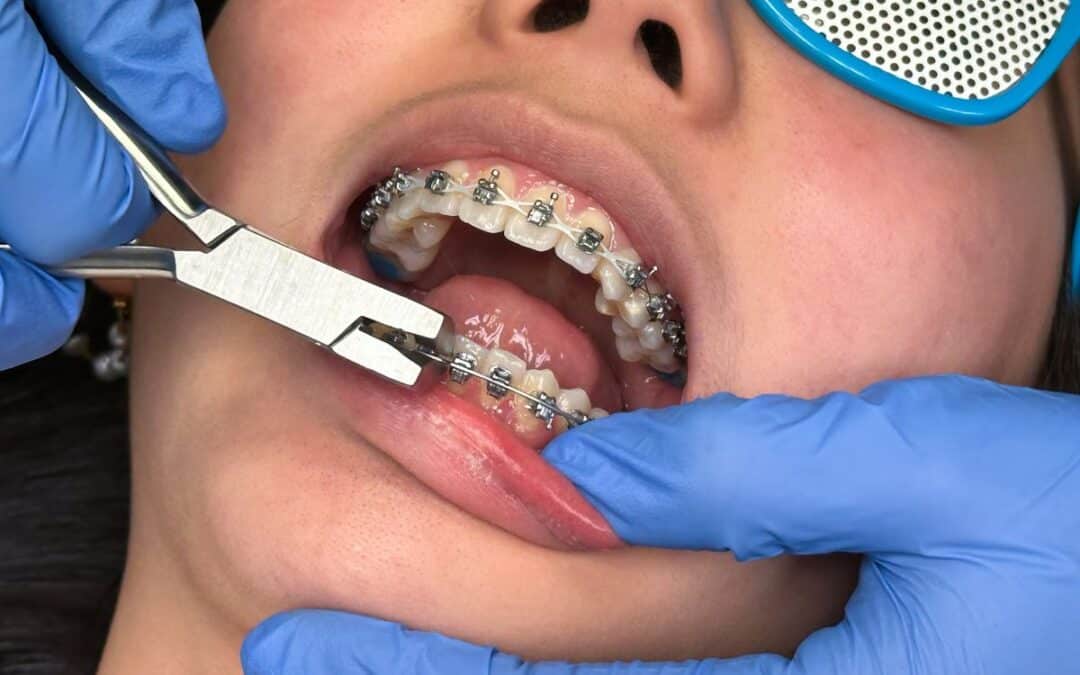
by 110 Dental & Orthodontics | Feb 20, 2026 | Braces, Orthodontics
Braces transform smiles by aligning teeth over time. Many patients, however, face a surprise: gums start bleeding more often during brushing or flossing. This change feels alarming but usually has straightforward explanations. With consistent care, most people see improvement quickly. Let’s break down the causes and share practical steps to restore comfort and health.
Understanding Gum Bleeding with Braces
Braces apply gentle pressure to move teeth. Gums respond to this shift with temporary sensitivity. The hardware also changes how you clean your mouth.
Food particles stick more easily around brackets and wires. Plaque builds up faster in those spots. Bacteria then irritate the gum tissue.
Gingivitis often develops as a result. It’s the early, reversible form of gum disease. Symptoms include redness, swelling, and bleeding. Research shows orthodontic patients experience higher rates of this due to cleaning difficulties.
Common Causes of Increased Bleeding
Hygiene challenges rank highest. Standard brushing misses areas near brackets. Flossing feels awkward at first.
Tightening appointments cause short-term soreness. Gums may bleed briefly after adjustments as tissues adapt.
Metal parts sometimes rub soft tissue. This leads to minor irritation or small abrasions.
Hormones influence gum reactions too. Growing teens often notice more sensitivity during treatment.
Dietary choices matter. Sugary or acidic items fuel bacteria and inflame gums further.
How Braces Impact Oral Health
Appliances create new surfaces for plaque. Complete removal becomes tougher without adapted techniques.
Bacteria release acids that harm gum tissue. Bleeding acts as an early warning sign from your body.
In places like Whitehouse, TX, patients getting braces in Whitehouse, TX benefit from local guidance on routines that prevent escalation. Consistent habits keep complications low.
Occasional tissue overgrowth around brackets appears. Known as hyperplasia, it typically resolves with better care.
Prevention Strategies for Healthier Gums
Switch to a soft-bristled brush. Hold it at a 45-degree angle to the gumline. Use gentle circular motions for full two minutes, twice a day.
Electric toothbrushes excel at reaching tight spaces. Their vibrations dislodge debris effectively.
Floss every day using threaders or water flossers. These tools glide under wires without hassle.
Add an antimicrobial mouthwash rinse. It cuts bacterial levels. Fluoride options also protect enamel.
Pick braces-friendly foods. Go for soft produce and avoid chewy or sticky treats.
Drink plenty of water. It naturally rinses particles and boosts saliva flow.
Addressing Yellow Stains on Braces Bands
Patients sometimes point out yellow stains on braces bands during visits. These often come from plaque or food pigments building up over time. A professional polish refreshes the look, and we can suggest small tweaks to your daily routine to keep them minimal moving forward.
When to Seek Professional Help
Bleeding that lingers beyond a week deserves attention. Contact your provider promptly.
Watch for infection signs like pus, fever, or severe swelling. Act quickly on these.
Regular professional cleanings every six months remove hidden buildup. They support your home efforts.
Trending FAQs on Gum Bleeding with Braces
Online searches reveal common concerns. Here are answers to frequently asked questions drawn from popular queries:
- Is it normal for gums to bleed when you first get braces? Yes, early bleeding is typical from adjustment pressure and initial irritation. It often calms within days with diligent care.
- How do I stop my gums from bleeding with braces? Focus on thorough brushing, daily flossing with tools, and mouthwash use. Persistent cases benefit from professional evaluation.
- Why do my gums bleed when I floss with braces? Flossing removes plaque that irritates already sensitive gums. Regular practice helps gums toughen and bleeding decrease.
- Can braces cause permanent gum damage? Rarely, with good hygiene. Untreated gingivitis might lead to recession, but prompt action usually prevents long-term issues.
- What toothpaste is best for bleeding gums with braces? Choose fluoride formulas with anti-gingivitis agents. Skip highly abrasive types that could damage hardware.
Statistics on Gum Health During Orthodontic Treatment
Key data from studies highlights the value of proactive steps:
| Issue |
Prevalence in Braces Wearers |
Notes |
| Gingival Inflammation |
Up to 70% in first year |
Tied to plaque around brackets; hygiene resolves most cases. |
| Bleeding on Probing |
50-60% increase |
Bacterial buildup main factor; cleanings lower risk. |
| Gingival Recession |
2-3% post-treatment |
Uncommon; linked to neglected care. |
| Plaque Accumulation |
40% higher than non-wearers |
Extra surfaces from braces; daily tools help control it. |
These numbers show why routines make a big difference. Early habits reduce risks sharply.
Additional Tips for Comfort
Apply orthodontic wax over sharp edges. It prevents rubbing.
Use approved pain relievers for soreness. Stick to recommended doses.
Gently massage gums with clean fingers after eating. It promotes circulation.
Note patterns in a simple journal. Share observations at check-ups.
If you are searching for an orthodontist near you in Whitehouse, TX, nearby experts offer tailored support for your specific situation.
Long-Term Benefits of Managing Gum Health
Good gum care now supports successful alignment later. Healthy tissues hold teeth in place better.
Fewer bleeding episodes keep treatment smooth. Progress continues without delays.
After braces, strong gums maintain your results. Retainers work more effectively.
Oral health ties to overall wellness. Protected gums lower risks for broader issues.
Build these habits today. They create benefits that last a lifetime.
Your orthodontic experience improves dramatically with attention to gum health. Small daily changes yield big rewards in comfort and results. Schedule an appointment, visit or give us a call—we’re here to help you every step of the way.







