by 110 Dental & Orthodontics | Apr 9, 2026 | Emergency Dental Care
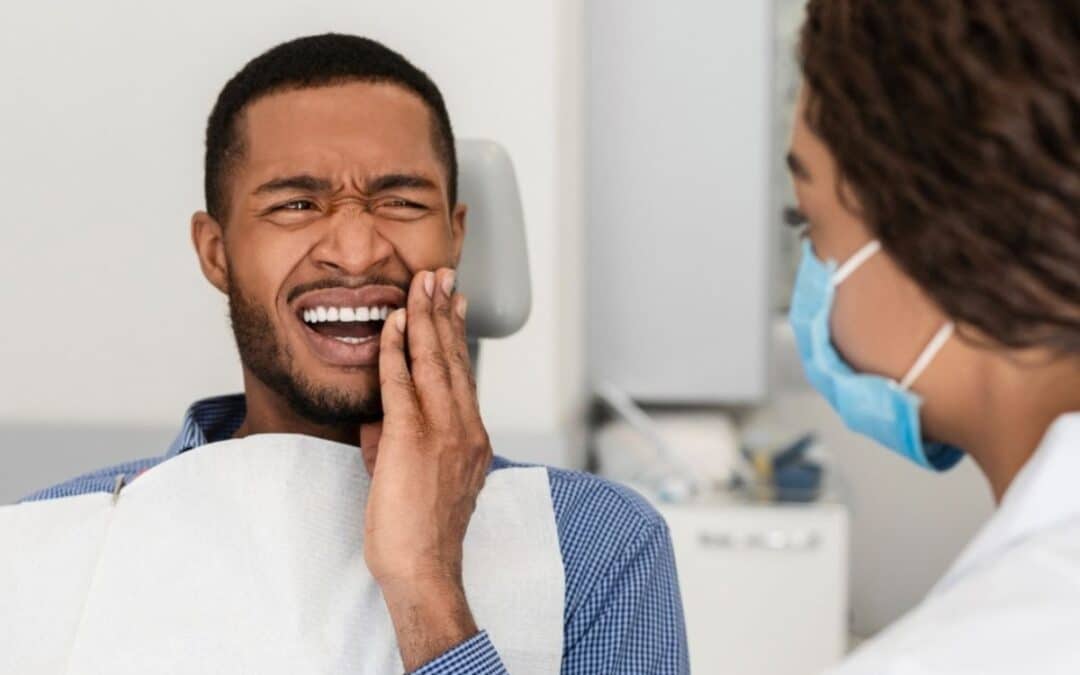
That sharp pressure in your upper teeth can stop you cold. One moment you feel fine, and the next an ache spreads across your cheek and jaw. Many people mistake this for a simple tooth problem. In reality, it often stems from inflamed sinuses pressing on nearby nerves. The confusion leaves you wondering what to do next. Relief starts with clear answers and the right steps forward.
Understanding Sinus Toothaches
Sinus toothaches happen when the maxillary sinuses swell. These air-filled spaces sit right above your upper back teeth. Inflammation from allergies, colds, or infections builds pressure. That pressure squeezes the roots of your molars and premolars. Pain feels dull and widespread. It often affects several teeth at once rather than one spot.
You might notice the ache worsens when you bend forward or lie down. Other signs include nasal congestion, facial tenderness, and postnasal drip. Unlike a cavity, the discomfort ties directly to sinus changes. Dental infections can also spread upward and create similar pressure. Either way, the pain disrupts sleep, work, and daily comfort.
How to Tell Sinus Pain from a True Dental Problem
Distinguishing the source matters for fast relief. Sinus pain stays vague and spreads. Dental pain usually stays sharp and local. Here is a quick comparison to guide you.
| Symptom |
Sinus Toothache |
Dental Toothache |
| Pain location |
Multiple upper teeth, cheeks, forehead |
One specific tooth |
| Pain type |
Dull ache, pressure |
Sharp, throbbing, or stabbing |
| Triggers |
Bending over, lying down |
Hot or cold foods, chewing |
| Other signs |
Runny nose, congestion, headache |
Swollen gums, visible decay, bad taste |
| Duration |
Comes with sinus symptoms |
May appear without nasal issues |
Use this table to track your symptoms. Note patterns over a day or two. Accurate notes help any professional reach the right diagnosis quickly.
When Should You Seek Emergency Dental Care?
Act fast if pain intensifies or lasts beyond a day. Seek care right away for swelling around the eyes or face, fever, or difficulty swallowing. These signs point to possible infection that needs prompt attention. Emergency teams evaluate quickly. They rule out dental sources first because untreated infections can worsen fast.
Waiting rarely helps. Early visits prevent complications and bring targeted relief. Professionals perform gentle exams and imaging when needed. They focus on your comfort from the first moment.
The Role of Emergency Dentistry in Sinus-Related Tooth Pain
Emergency dentistry shines in these confusing cases. Dentists examine teeth and surrounding tissues with care. They use X-rays to check for hidden dental issues like abscesses or cracks. If the problem starts in a tooth, they provide immediate relief steps. If sinuses appear responsible, they guide you toward the right medical follow-up.
This clear process removes guesswork. You leave with a plan instead of lingering doubt. Local expertise makes the difference in timely care. Consulting with our emergency dentist in Whitehouse delivers that precise evaluation many need.
Simple Steps for Relief While You Wait
You can ease discomfort at home while arranging care. Drink plenty of water to thin mucus. Run a humidifier to moisten the air. Try warm compresses on your cheeks for ten minutes at a time. Saline nasal rinses clear passages gently. Over-the-counter decongestants help short term, but follow package directions closely.
Avoid extreme temperatures in food or drink. Rest with your head elevated. These actions reduce pressure and buy time until professional help arrives. They work best alongside proper diagnosis.
Trending FAQs
- Can a sinus infection cause a toothache? Yes. Inflammation in the maxillary sinuses presses on upper tooth roots and creates tooth-like pain.
- How do I know if my tooth pain comes from sinuses or teeth? Sinus pain affects several upper teeth and worsens with head position changes. Dental pain stays sharp and local to one tooth with sensitivity to temperature or biting.
- What relieves sinus tooth pain quickly? Hydration, humidifiers, saline rinses, and warm compresses reduce pressure. Professional evaluation confirms the cause.
- When should I see a dentist for sinus toothache? See one immediately if pain lasts over 24 hours, swelling appears, or fever develops.
- Can an emergency dentist help if sinuses cause the pain? Yes. They diagnose the source accurately and coordinate care if referral is needed.
- Does tooth infection ever spread to sinuses? Yes. Upper tooth infections can trigger sinus problems. Early dental care stops the spread.
Protecting Your Smile Long Term
Prevention keeps both sinus and dental issues at bay. Brush and floss daily with gentle technique. Stay current with routine check-ups. Manage allergies before they inflame sinuses. Address small dental concerns before they grow. These habits build resilience and reduce surprise pain episodes.
If you are searching for a dentist near you, expert evaluation brings quick answers and lasting comfort when symptoms arise.
Sinus toothaches prove tricky yet manageable with the right approach. You deserve clear answers and swift relief. Knowledge turns confusion into confidence. Take the next step toward comfort and peace of mind. Reach out today to schedule an appointment.

by 110 Dental & Orthodontics | Sep 15, 2025 | Emergency Dental Care
Have you ever felt a sharp, unrelenting pain in your mouth that disrupts your day? It’s more than an annoyance. This could signal a serious issue needing prompt care. Let’s explore why addressing it right away matters for your health.
Understanding an Abscessed Tooth
An abscess forms when bacteria invade the tooth’s inner layers. Pus builds up, creating pressure. This often stems from untreated decay or injury.
What Causes It?
Decay is a top culprit. Cracks let germs in. Past dental work can fail, too. Trauma from accidents plays a role. Poor hygiene speeds the process.
Recognizing the Signs
Pain throbs intensely. Swelling appears in the gums or face. Fever might hit. Lymph nodes enlarge. A bad taste lingers. Sensitivity spikes with hot or cold. Chewing hurts badly. In some cases, issues like broken braces can lead to infections, mimicking symptoms of an orthodontic emergency. Watch for these red flags.
The Risks of Delaying Treatment
Ignoring the problem worsens it. Infection spreads fast. It can reach the jawbone. Sinuses get involved. Brain risks rise in rare cases.
Bone loss occurs over time. Teeth may loosen. Sepsis is a real threat. This blood infection demands hospital care. Heart issues link to oral bacteria. Delaying invites these dangers.
| Complication |
Potential Impact |
Likelihood if Untreated |
| Jawbone Infection |
Bone weakening, possible surgery |
High (over 50% in advanced cases) |
| Sepsis |
Life-threatening systemic response |
Moderate (5-10% without care) |
| Tooth Loss |
Permanent gap, shifting teeth |
Very High (up to 80%) |
| Sinus Issues |
Chronic pain, breathing problems |
Common (30-40%) |
| Heart Complications |
Increased risk of endocarditis |
Low but serious (1-2%) |
Stats show untreated cases often lead to emergencies. Don’t let it escalate.
Treatment Options Available
Drainage relieves pressure first. Antibiotics fight bacteria. Root canals save the tooth. Extraction happens if needed. Follow-up prevents recurrence.
Pain relief comes quick after action. Healing starts soon. Modern methods make it comfortable. Expect a smooth process with skilled pros.
Prevention Strategies for Better Oral Health
Brush twice daily. Floss regularly. Use mouthwash. Visit our emergency dentist in Whitehouse, TX, for checkups. Avoid sugary foods. Protect teeth in sports.
Healthy habits cut risks. Early spots catch issues. Stay vigilant.
Trending FAQs on Abscessed Tooth
Here are common questions people ask on Google about this topic, with clear answers:
- What are the first signs of an abscessed tooth?
Early signs include persistent pain, swelling around the gum, and sensitivity to temperature changes. A pimple-like bump may form on the gum.
- Can an abscessed tooth heal on its own?
No, it won’t resolve without intervention. The infection persists and can spread, requiring professional drainage and antibiotics.
- Is an abscessed tooth considered a dental emergency?
Yes, especially with severe pain, fever, or swelling. Prompt care prevents complications like infection spread.
- How long can you go with an untreated abscessed tooth?
Avoid waiting at all. Symptoms may worsen in days, leading to serious health risks within weeks if ignored.
- What home remedies help with abscessed tooth pain?
Rinse with saltwater for temporary relief. Apply a cold compress to reduce swelling. But these aren’t substitutes for dental treatment.
These address frequent concerns based on search trends.
In East Texas areas like Whitehouse, locals often face these issues due to active lifestyles. Seeking timely help from an emergency dentist in Whitehouse, TX, makes a difference. It ensures quick recovery.
If you are searching for an “emergency dentist near me“, know that expert care is close by. Acting fast eases worries.
Facing this challenge? Reach out today. Call (903)-328-6577 to schedule an appointment. Your smile deserves protection. Stay healthy.
by 110 Dental & Orthodontics | Aug 6, 2025 | Emergency Dental Care
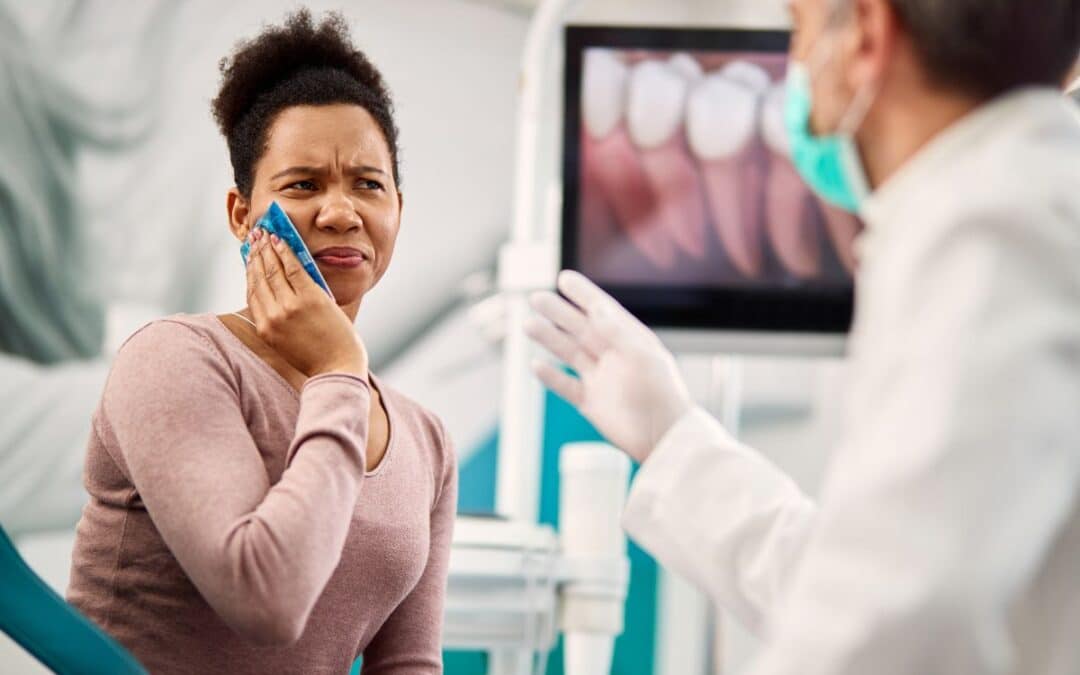
Have you ever woken up with a puffy face or sore mouth during peak pollen season? Many people dismiss these as typical allergy woes, but they might signal something more tied to your smile. This connection often surprises folks, yet understanding it can ease discomfort and protect your health. Let’s explore how everyday allergens could spark unexpected oral reactions.
Understanding Allergies and Their Impact on Oral Health
Allergies happen when your immune system overreacts to harmless substances like pollen, dust, or food. This response releases chemicals that cause inflammation. In the mouth, that means potential issues for teeth and gums.
Sinus cavities sit close to the upper tooth roots. When allergens irritate them, pressure builds up. This can mimic tooth problems. Dry mouth often follows, as mouth breathing dries saliva. Saliva fights bacteria, so less of it raises cavity risks.
Gum tissues react, too. Inflammation from histamines can make them tender. Postnasal drip adds bacteria, worsening breath, and irritation. Overall, allergies disrupt oral balance.
Common Ways Allergies Cause Swelling in the Mouth
Swelling stems from the body’s fight against allergens. Oral allergy syndrome hits fast after eating certain fruits or veggies in pollen-sensitive people. Lips, tongue, and throat puff up, sometimes reaching gums.
More severe cases involve anaphylaxis. This rare reaction swells the entire mouth area, blocking airways. Seek help immediately if breathing gets hard.
Every day, allergies inflame sinuses, pressing on facial nerves. Gums might redden and enlarge. Tooth sensitivity spikes from exposed roots. These effects vary by person and allergen strength.
Differentiating Allergy Swelling from Dental Infections
Not all swelling points to allergies. Infections like abscesses cause sharp pain and pus. Allergies bring itchiness or a runny nose.
Timing helps. Seasonal flares match pollen counts. Food triggers link to meals. Dental issues persist without these cues.
If unsure, note symptoms. Allergy pain often affects multiple teeth. True dental problems focus on one spot. Tracking helps pinpoint causes.
Swelling from allergies might resolve with antihistamines. Persistent cases need professional checks to rule out infections.
When Swelling Becomes a Dental Emergency
Sudden, intense puffiness demands quick action. It could stem from severe reactions needing urgent care. In areas like Whitehouse, handling a dental emergency in Whitehouse, TX, ensures prompt relief from qualified experts.
Ignore it, and complications arise. Swollen tissues hinder eating or speaking. Bacteria thrive in inflamed spots, risking further issues.
Watch for red flags: difficulty swallowing, fever, or rapid spread. These signals escalate beyond home remedies.
Trending FAQs on Allergies and Dental Swelling
People often search for clarity on this topic. Here are some frequently asked questions based on common online queries:
- Can allergies cause tooth pain? Yes, sinus pressure from inflammation presses on tooth roots, creating an ache or sensitivity.
- How do seasonal allergies affect gums? They trigger inflammation, leading to redness, swelling, and discomfort in gum tissues.
- Can allergies lead to dry mouth? Absolutely, mouth breathing and medications reduce saliva, increasing decay risks.
- Does oral allergy syndrome cause severe swelling? It can swell lips and throat quickly, though usually mild unless anaphylaxis occurs.
- How to tell if tooth pain is from allergies or infection? Allergies often come with nasal symptoms; infections bring localized throbbing and fever.
These address key concerns, drawing from widespread searches.
Statistics on Allergies and Oral Health Impacts
Allergies affect millions, with oral issues often overlooked. Here’s a quick table of relevant stats:
| Statistic |
Detail |
Source Insight |
| Allergy Prevalence |
Over 50 million Americans face seasonal allergies yearly |
Asthma and Allergy Foundation of America |
| Dry Mouth from Meds |
Up to 40% of antihistamine users report reduced saliva |
Dental research studies |
| Sinus-Related Tooth Pain |
Affects 20-30% of allergy sufferers during peaks |
Clinical observations |
| Severe Reactions |
Anaphylaxis hits 1 in 50 people lifetime |
Allergy organizations |
These numbers highlight why awareness matters.
Prevention Tips for Allergy-Related Dental Issues
Stay ahead with simple steps. Identify triggers through testing. Avoid known allergens like certain pollens or foods.
Use saline rinses to clear sinuses. This reduces pressure on teeth. Hydrate well to combat dry mouth.
Brush gently twice daily. Floss to remove trapped particles. Antihistamines help, but choose non-drying types.
Regular checkups catch early signs. Cleanings remove buildup that worsens inflammation.
For sensitivity, try desensitizing toothpaste. It shields nerves from triggers.
Management Strategies for Relief
- When symptoms hit, act fast. Over-the-counter decongestants ease sinus swelling.
- Warm compresses soothe facial puffiness. Apply for 10-15 minutes.
- Gargle salt water to reduce throat and gum irritation. It draws out excess fluid.
- If breathing issues arise, use prescribed epinephrine. Follow up with care.
- Combine these for better outcomes. Track what works for future flares.
- In tough spots, an emergency dentist near you can offer expert guidance on swelling tied to allergies.
Long-Term Oral Health Protection Amid Allergies
- Build habits that last. Maintain humidity to prevent dry air from worsening symptoms.
- Opt for allergy-proof bedding. This cuts dust mite exposure.
- Exercise boosts immunity, potentially easing reactions.
- Pair with a balanced diet. Nutrients support gum health against inflammation.
- Consistency pays off. Fewer flares mean healthier smiles.
As we wrap up, remember that allergies and oral health intertwine more than most realize. Addressing them head-on brings comfort and confidence. If you notice persistent swelling or pain, don’t wait. Reach out for support. And if you are searching for an emergency dentist serving near Whitehouse and surrounding communities, call (903)-328-6577 to schedule an appointment today. Your smile deserves swift, caring attention.

by 110 Dental & Orthodontics | Feb 26, 2025 | Emergency Dental Care
Your teeth are protected by a tough outer layer called enamel. This is the hardest substance in the human body, designed to shield your teeth from the wear and tear of daily activities like chewing, speaking, and brushing. However, enamel is not indestructible; over time, it can wear away due to various factors. This is known as enamel erosion, a common dental issue that can lead to sensitivity, discoloration, and increased vulnerability to cavities.
In this blog, we’ll explore enamel erosion, why it happens, and how to prevent it from affecting your smile. If you’re experiencing symptoms of enamel erosion, it’s essential to consult a professional, such as an Emergency Dentist in Whitehouse, to get timely advice and treatment.
What is Enamel Erosion?
Enamel erosion occurs when the protective outer layer of your teeth wears away, exposing the underlying dentin, which can lead to tooth sensitivity and discomfort. The enamel is composed mainly of minerals; when it is damaged or eroded, it doesn’t regenerate. The lost enamel can’t grow back, making prevention and early intervention crucial.
Common Causes of Enamel Erosion
Several factors contribute to enamel breakdown; understanding these causes can help avoid damage. Here are the most common reasons why enamel erosion occurs:
1. Acidic Foods and Beverages
One of the primary causes of enamel erosion is the consumption of acidic foods and drinks. Citrus fruits like oranges, lemons, grapefruits, and carbonated beverages like soda and sparkling water contain high levels of acid that can weaken enamel. Over time, frequent exposure to these acids can cause enamel to dissolve.
2. Acid Reflux
Gastroesophageal reflux disease (GERD) is another culprit. This condition causes stomach acids to flow back into the mouth, which can gradually erode tooth enamel. People with chronic acid reflux or heartburn may experience enamel erosion more rapidly.
3. Brushing Too Hard
While brushing your teeth is essential for good oral hygiene, brushing with excessive force can be detrimental. Using a hard-bristled toothbrush or brushing too vigorously can damage enamel and lead to gum recession. Using a soft-bristled brush and gentle strokes is important to avoid unnecessary wear on your enamel.
4. Dry Mouth
Saliva plays a critical role in protecting your teeth from enamel erosion. It neutralizes acids in the mouth, helping to remineralize enamel. When there’s a reduction in saliva production, often due to medications or certain medical conditions, the risk of enamel erosion increases. A dry mouth allows acids to remain in the mouth longer, accelerating enamel breakdown.
5. Bruxism (Teeth Grinding)
Grinding your teeth, often done unknowingly during sleep, can cause wear on the enamel. Over time, the pressure from grinding can contribute to enamel thinning and damage. If you notice signs of teeth grinding, such as jaw pain or worn-down teeth, you must seek professional help from your dentist.
6. Sugar and Carbohydrate Consumption
Sugar and refined carbohydrates provide food for harmful bacteria in the mouth. When these bacteria feed on sugars, they produce acids that can erode enamel. Frequent snacking on sugary foods, especially between meals, can lead to enamel breakdown.
Symptoms of Enamel Erosion
Enamel erosion can manifest in several ways. Some of the most common signs include:
- Tooth Sensitivity: You may experience discomfort or pain when eating hot, cold, sweet, or acidic foods.
- Discoloration: As enamel wears away, the yellowish dentin beneath it becomes more visible, causing your teeth to appear more yellow.
- Rough or Transparent Edges: The edges of your teeth may begin to look translucent or rough as enamel thins.
- Cracks and Chips: Weakened enamel may cause your teeth to become more prone to damage, including cracks and chips.
How to Prevent Enamel Erosion?
Preventing enamel erosion is essential to maintaining healthy teeth and gums. Here are some practical tips to protect your enamel:
1. Limit Acidic Foods and Drinks
Cut back on foods and beverages that are high in acid, such as citrus fruits, soda, wine, and coffee. When you do consume acidic items, try drinking water afterward to neutralize the acid in your mouth.
2. Brush with the Right Technique
Brush your teeth with a soft-bristled toothbrush and gentle, circular motions. Avoid brushing immediately after eating acidic foods, as this can make enamel more vulnerable. Wait at least 30 minutes to allow your mouth to return to a neutral pH.
3. Use Fluoride Toothpaste
Fluoride helps to strengthen enamel and can slow down the erosion process. Make sure to use fluoride toothpaste and consider rinsing with a fluoride mouthwash to further protect your teeth.
4. Stay Hydrated
Drink plenty of water to ensure your mouth stays moist and your saliva production remains at healthy levels. This will help neutralize acids and wash away food particles that can contribute to enamel erosion.
5. Wear a Mouthguard
If you grind your teeth at night, consider wearing a mouthguard. This can help protect your teeth from the pressure and prevent enamel wear caused by bruxism.
6. Visit Your Dentist Regularly
Regular dental checkups are essential for monitoring the condition of your enamel. If you’re experiencing symptoms of enamel erosion, an Emergency Dentist in Whitehouse can help assess the damage and suggest treatment options to restore and protect your teeth.
Conclusion
Enamel erosion is a common problem, but it’s also preventable with the proper precautions. By understanding the causes and symptoms of enamel erosion, you can take proactive steps to protect your smile. If you’re experiencing signs of enamel damage, don’t wait until the situation worsens—reach out to a Dentist in Whitehouse to discuss your options. For more information or to schedule an appointment, contact us today!

by 110 Dental & Orthodontics | Feb 12, 2025 | Emergency Dental Care
Orthodontic treatment is a journey toward a straighter, healthier smile, but sometimes unexpected issues arise. While minor discomfort is normal with braces or aligners, certain problems require urgent attention. Knowing the symptoms of an orthodontic emergency can help you act quickly and prevent further complications. If you ever find yourself in severe pain or dealing with a broken orthodontic appliance, reaching out to an emergency dentist can make all the difference.
What Is an Orthodontic Emergency?
An orthodontic emergency is any situation involving braces, aligners, or other orthodontic appliances that cause significant pain, difficulty in daily functions, or a risk of injury. While not every issue requires immediate professional intervention, some symptoms should never be ignored.
Common orthodontic emergencies include:
- Severe pain or discomfort that doesn’t go away
- Broken brackets or wires that cause irritation
- Swelling, infection, or abscesses in the mouth
- Difficulty eating, speaking, or breathing due to orthodontic devices
Recognizing the signs of an emergency can help you take quick action to protect your teeth and oral health.
Key Symptoms of an Orthodontic Emergency
1. Severe or Persistent Pain
Mild soreness is normal when wearing braces or aligners, especially after an adjustment. However, if you experience intense pain that doesn’t subside with over-the-counter pain relievers, it could indicate a serious issue. Possible causes include:
- A misaligned appliance putting pressure on teeth and gums
- An infection developing beneath the gums
- A broken wire or bracket causing injury inside the mouth
If the pain is unbearable or lasts more than a couple of days, seeking help from an emergency dentist in Whitehouse is essential.
2. Broken Brackets or Protruding Wires
Brackets and wires are crucial for guiding teeth into alignment. If a bracket becomes loose or completely detaches, it can delay treatment and cause irritation. A broken or protruding wire can also lead to painful cuts or sores inside the mouth. While orthodontic wax can provide temporary relief, professional repair is necessary as soon as possible.
3. Swelling, Infections, or Abscesses
Swelling, pus, or a persistent fever can indicate a serious infection, which should never be ignored. Common causes include:
- Food trapped around braces leads to bacterial buildup
- A damaged appliance causing irritation and infection
- A pre-existing dental issue that worsens due to orthodontic treatment
If you notice signs of infection, it’s important to see a dentist immediately to prevent further complications.
4. Difficulty Eating, Speaking, or Breathing
Orthodontic appliances should never interfere with essential functions like eating, speaking, or breathing. If you find it difficult to chew food, close your mouth properly, or breathe comfortably, you may be dealing with an improperly fitted appliance. This requires urgent evaluation by an orthodontist to prevent further issues.
5. Sores or Ulcers That Won’t Heal
Braces can sometimes cause minor sores inside the mouth. However, if you develop large, painful ulcers that don’t heal within two weeks, this could be a sign of excessive friction from the appliance or an allergic reaction. If the discomfort persists, it’s best to consult a professional.
What to Do in an Orthodontic Emergency
If you suspect an orthodontic emergency, follow these steps to minimize discomfort and prevent further damage:
- Assess the severity: If you’re experiencing extreme pain, bleeding, or breathing issues, seek emergency dental care immediately.
- Use orthodontic wax: If a bracket or wire is irritating your mouth, covering it with wax can provide temporary relief.
- Take pain relievers: Over-the-counter medications like ibuprofen can help manage pain while you wait for professional care.
- Rinse with salt water: This can help reduce swelling and prevent infection if there’s an open wound in your mouth.
- Call your orthodontist: If the issue isn’t life-threatening but still concerning, schedule an appointment as soon as possible.
Conclusion
While orthodontic treatment is designed to improve your smile, emergencies can happen. Severe pain, broken appliances, infections, or difficulty eating and breathing are signs that require immediate attention. If you experience any of these symptoms, don’t hesitate to seek professional help. Consulting an orthodontist in Whitehouse can ensure your treatment stays on track while keeping your oral health in check. Remember, taking quick action in an orthodontic emergency can prevent long-term complications and help you maintain a healthy, confident smile.
by 110 Dental & Orthodontics | Jan 14, 2025 | Emergency Dental Care
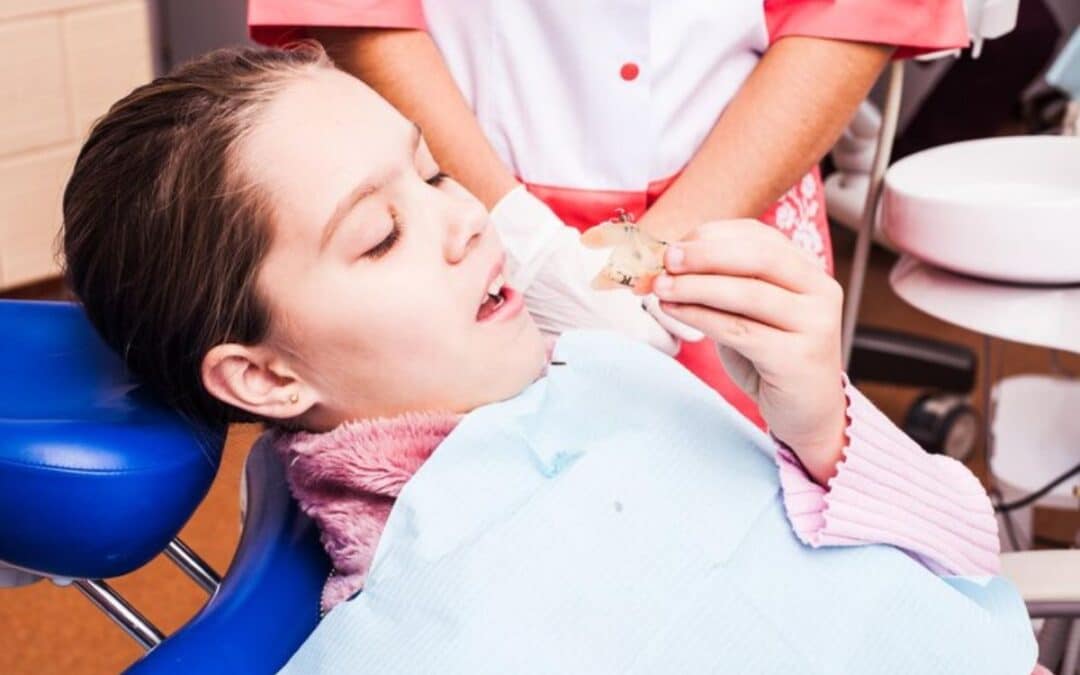
Teenagers lead active, busy lives filled with sports, social activities, and school responsibilities. While this stage of life is exciting, it can sometimes lead to unexpected dental emergencies. Knowing how to recognize and address these situations can prevent long-term oral health problems and ensure your teen’s smile stays bright. Here’s a guide to understanding the most common dental emergencies teenagers face and how to handle them effectively.
Common Dental Emergencies in Teenagers
Teenagers are especially prone to dental emergencies due to their active lifestyles. Here are some of the most frequent issues:
- Knocked-Out Teeth: Sports injuries or accidental falls can cause a tooth to be completely dislodged. Acting quickly can often save the tooth.
- Chipped or Broken Teeth: Biting hard objects or impacts to the face can result in chipped or fractured teeth, which may expose nerves and cause pain.
- Severe Toothaches: Persistent tooth pain could indicate deep cavities, infections, or other underlying problems.
- Lost Fillings or Crowns: Teens with prior dental work might lose a filling or crown, exposing sensitive areas of the tooth.
- Orthodontic Emergencies: For those with braces, loose wires or broken brackets can lead to discomfort or injuries to the soft tissues in the mouth.
When these emergencies occur, seeking prompt care from an emergency dentist in Whitehouse is crucial to minimize further complications.
What to Do in a Dental Emergency
When your teenager encounters a dental emergency, staying calm and knowing what to do can make all the difference. Here are five essential steps to follow:
- For Knocked-Out Teeth: Rinse the tooth gently with water, being careful not to touch the root. If possible, place it back in its socket or store it in milk to keep it moist until you can see a dentist.
- For Chipped or Broken Teeth: Rinse the mouth with warm water, apply a cold compress to reduce swelling, and collect any broken fragments to bring to the dentist.
- For Toothaches: Rinse with warm salt water, and use a cold compress to alleviate discomfort. Avoid applying aspirin directly to the gums, as it can cause irritation.
- For Orthodontic Issues: Cover sharp wires with orthodontic wax to protect the gums and cheeks until an appointment can be arranged.
- For Lost Fillings or Crowns: Apply dental cement (available at most pharmacies) to the area as a temporary fix and schedule a visit with your dentist promptly.
Preventing Dental Emergencies in Teenagers
Prevention is always better than cure. Here’s how to help your teenager minimize the risk of dental emergencies:
- Wear Mouthguards: Custom-fitted mouthguards during sports activities protect teeth from impact injuries.
- Practice Good Oral Hygiene: Brushing and flossing regularly can prevent cavities and gum disease, reducing the risk of pain or infections.
- Avoid Hard Foods: Teach your teen to avoid chewing on ice, popcorn kernels, or other hard objects.
- Use Teeth Properly: Teeth are for chewing, not opening packages or cracking nuts.
- Attend Regular Dental Checkups: Routine visits to the dentist ensure that potential issues are caught early before they escalate.
When to Seek Professional Help
Not all dental issues are emergencies, but it’s vital to know when professional care is necessary. Here are five signs it’s time to call a dentist:
- Persistent or severe tooth pain that doesn’t improve with over-the-counter remedies.
- Swelling in the face or gums that could indicate an infection.
- A knocked-out tooth, as quick action can increase the chances of saving it.
- Bleeding that doesn’t stop after applying pressure for 15 minutes.
- A visible abscess or pus around a tooth or gum line.
If your teen experiences any of these, contacting an emergency dentist in Whitehouse promptly is essential to address the problem and prevent further complications.
Handling Teen Dental Emergencies with Confidence
Knowing how to recognize and respond to dental emergencies ensures that your teenager’s oral health remains a priority. Whether it’s equipping them with a mouthguard or educating them about good oral hygiene, prevention plays a significant role. And when an emergency does arise, having access to a trusted local dentist near you will make all the difference in ensuring a swift and stress-free recovery.








