
by 110 Dental & Orthodontics | Jul 17, 2025 | Dental Implants, Veneers
Choosing between dental implants and veneers can feel overwhelming. Both options promise a brighter, more confident smile, but which one suits women best? This blog dives into the differences, benefits, and considerations to help you make an informed decision. Whether you’re seeking durability or a quick aesthetic fix, we’ll explore what works for your lifestyle and dental needs.
Understanding Dental Implants
Dental implants are a long-term solution for missing teeth. They involve a titanium post surgically placed into the jawbone, acting as a tooth root. A custom crown is then attached, mimicking a natural tooth. Implants are sturdy, functional, and blend seamlessly with your smile. They’re ideal for women who want a permanent fix that feels natural.
Implants require a healthy jawbone and good oral health. The process takes several months, including healing time. However, the result is a durable tooth replacement that can last decades with proper care. Women often choose implants for their reliability and ability to restore full chewing function.
Exploring Dental Veneers
Veneers are thin, custom-made shells bonded to the front of your teeth. They’re designed to enhance aesthetics, covering imperfections like stains, chips, or gaps. Made from porcelain or composite resin, veneers offer a quick transformation, often completed in just a couple of visits. They’re popular among women seeking a radiant smile for social or professional reasons.
Unlike implants, veneers don’t replace missing teeth. They’re best for cosmetic enhancements rather than functional restoration. Veneers require minimal tooth enamel removal, making them less invasive. However, they may need replacement every 10-15 years, depending on wear and tear.
Key Differences Between Implants and Veneers
Purpose and Functionality
Implants address missing teeth, restoring both function and appearance. They’re a go-to for women who’ve lost a tooth due to injury or decay. Veneers, on the other hand, focus on aesthetics. They’re perfect for covering surface flaws, but don’t replace teeth. If you need dental implants in Whitehouse, TX, consult a trusted dentist to assess your needs.
Durability and Longevity
Implants are built to last. With proper care, they can endure a lifetime, making them a favorite for women seeking permanence. Veneers, while durable, typically last 10-20 years. Lifestyle factors like teeth grinding or acidic diets can shorten their lifespan. Regular check-ups help maintain both options.
Procedure and Recovery
Implants involve surgery, requiring a longer recovery period. The process includes consultations, surgery, and follow-ups. Veneers are less invasive, with minimal discomfort and quicker results. For women with busy schedules, veneers might seem more appealing due to the shorter timeline.
Health Considerations for Women
Women’s dental health can be influenced by unique factors like hormonal changes or pregnancy. These can affect gum health, which is critical for implants. For instance, sinus issues due to dental implants can occur if upper jaw implants are near sinus cavities, requiring careful planning by your dentist. Veneers, being surface-level, don’t typically pose such risks but may not suit women with severe tooth damage.
Bone density is another consideration. Women, especially post-menopause, may experience bone loss, impacting implant eligibility. Your dentist will evaluate your jawbone health to ensure implants are viable. Veneers don’t require bone support, making them a versatile option for cosmetic fixes.
Aesthetic Outcomes for Confidence
Both implants and veneers boost confidence, but in different ways. Implants provide a natural look and feel, ideal for women wanting a seamless smile. Veneers offer a Hollywood-worthy transformation, perfect for those prioritizing aesthetics. If you’re aiming for a polished look for events or daily life, veneers might edge out. However, implants shine for overall functionality.
Lifestyle Compatibility
Your lifestyle plays a big role in this decision. Active women who enjoy sports or crunchy foods may prefer implants for their strength. Veneers require caution with hard foods to avoid chipping. If you’re a coffee or wine enthusiast, veneers resist stains better than natural teeth, but implants with porcelain crowns are equally stain-resistant.
If you are searching for a dentist serving in Whitehouse, TX, and surrounding communities, finding one experienced in both procedures is key. They can guide you based on your daily habits and long-term goals.
Trending FAQs on Dental Implants vs. Veneers
Here are answers to common questions women ask about implants and veneers, sourced from popular Google queries:
-
Can veneers fix crooked teeth?
Veneers can mask mild misalignment, creating the appearance of straighter teeth. However, they don’t correct the underlying position. Orthodontics or implants may be better for functional alignment issues.
-
Are dental implants painful?
The procedure involves local anesthesia, so discomfort is minimal during surgery. Post-procedure soreness is manageable with prescribed medications. Most women report mild discomfort during recovery.
-
How long do veneers last compared to implants?
Veneers typically last 10-20 years, while implants can last a lifetime with proper care. Maintenance, like regular cleanings, extends the life of both.
-
Can anyone get dental implants?
Not everyone is a candidate. Healthy gums and sufficient jawbone density are necessary. Women with certain health conditions may need alternative solutions like veneers.
-
Do veneers ruin your teeth?
Veneers require minimal enamel removal, which is irreversible but doesn’t “ruin” teeth if done properly. A skilled dentist ensures the process is safe.
Maintenance and Care Tips
Implants require diligent oral hygiene, similar to natural teeth. Brush twice daily, floss, and attend regular dental check-ups. Veneers also need care to prevent staining or damage. Avoid biting hard objects, and use a mouthguard if you grind your teeth. Both options benefit from a consistent oral care routine to maintain their look and function.
Making the Right Choice
Choosing between implants and veneers depends on your goals. Want a permanent fix for missing teeth? Implants are likely your best bet. Seeking a quick cosmetic upgrade? Veneers could be the answer. Discuss your options with a dentist to align the choice with your dental health and lifestyle.
Your Smile, Your Choice
Your smile is a powerful asset, and whether you choose dental implants or veneers, the goal is a confident, healthy you. Both options offer unique benefits tailored to different needs. Take the first step by consulting a trusted dentist to explore what’s right for you. To schedule an appointment, call (903) 328-6577 and start your journey to a radiant smile today.
by 110 Dental & Orthodontics | Jun 4, 2025 | Dental Implants
Dental implants have become a go-to solution for replacing missing teeth, offering a natural look and long-lasting functionality. For Whitehouse, TX, residents living with diabetes, the journey to a restored smile can come with unique considerations. This blog will explore how diabetes impacts the dental implant process, what precautions to take, and how to ensure a successful outcome. Let’s dive into the essentials to help you make informed decisions about your oral health.
Understanding Dental Implants and Diabetes
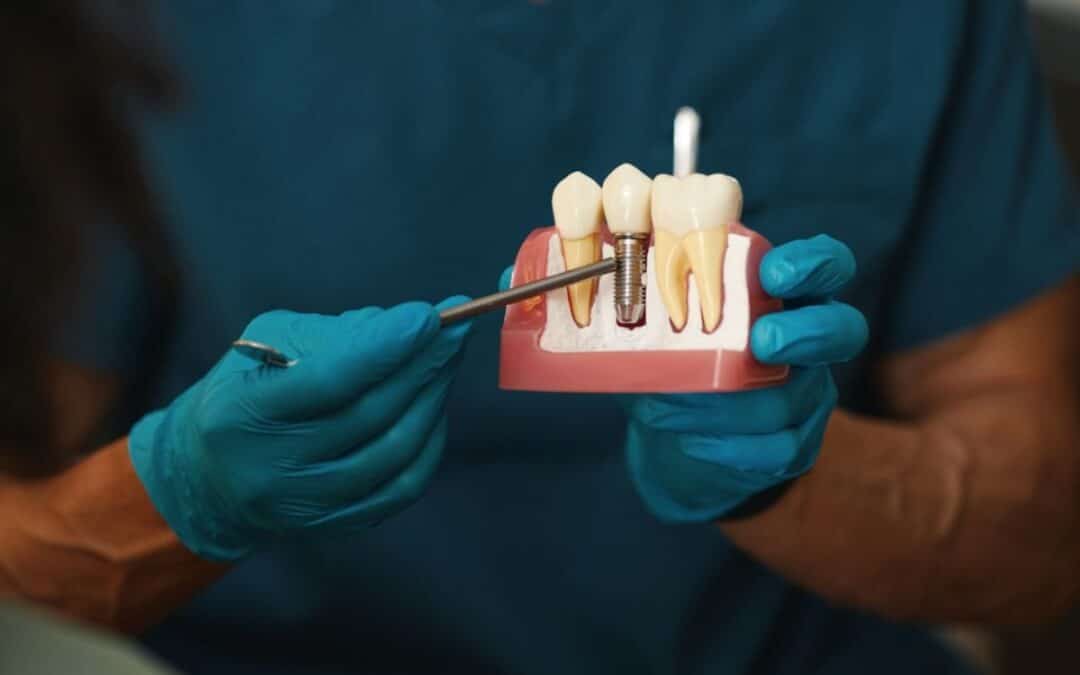
Dental implants are titanium posts surgically placed into the jawbone to act as artificial tooth roots. They support crowns, bridges, or dentures, mimicking natural teeth in both appearance and function. For diabetics, the process can be more complex due to the condition’s effect on healing and infection risk. High blood sugar levels can slow recovery and increase the likelihood of complications like gum disease or implant failure. However, with proper management, many diabetics successfully receive implants. The key lies in controlling blood glucose levels and working closely with your healthcare team.
Can Diabetics Get Dental Implants?
Absolutely, diabetics can get dental implants, but careful planning is essential. Studies, such as those from the American Academy of Implant Dentistry, show that well-controlled diabetics have success rates comparable to non-diabetics, often above 95%. The primary concern is poor glycemic control, which can impair osseointegration, the process where the implant fuses with the jawbone. Uncontrolled diabetes may also heighten the risk of peri-implantitis, a gum infection around the implant. If your A1C levels are stable (typically below 7%) and you maintain good oral hygiene, you’re likely a strong candidate. Always consult your endocrinologist and dentist to assess your readiness.
Steps to Ensure a Successful Implant Journey in Whitehouse
For Whitehouse residents considering this procedure, preparation is critical. Here’s how to set yourself up for success:
- Manage Blood Sugar: Keep your glucose levels in check before and after surgery. Consistent monitoring and medication adherence are vital.
- Prioritize Oral Hygiene: Brush twice daily, floss regularly, and use an antiseptic mouthwash to reduce infection risks.
- Choose an Experienced Dentist: Look for professionals in dental implants in Whitehouse, TX, who have experience working with diabetic patients. Their expertise can make a significant difference.
- Follow Pre- and Post-Surgery Guidelines: Your dentist may recommend antibiotics before surgery to prevent infection. After the procedure, stick to a soft diet and avoid smoking, which can delay healing.
- Schedule Regular Checkups: Frequent dental visits help catch potential issues early, ensuring your implant remains stable.
These steps, combined with a tailored treatment plan, can help mitigate risks and support a smooth recovery.
How Diabetes Affects Healing and Implant Longevity
Diabetes can slow the body’s natural healing process, which is crucial for implant success. Elevated blood sugar levels reduce blood flow, impairing the delivery of oxygen and nutrients to the surgical site. This can delay osseointegration and increase the chance of infection. Additionally, diabetics are more prone to gum disease, which can compromise the implant’s stability over time. However, with diligent care, these risks can be minimized. Maintaining a healthy diet, managing stress, and following your dentist’s advice can enhance healing and ensure your implant lasts for decades.
Lifestyle Tips for Diabetics with Dental Implants
Living with implants as a diabetic requires ongoing care. Adopt a balanced diet low in sugars to support both your implants and overall health. Foods rich in calcium and vitamin D, like leafy greens and dairy, strengthen jawbone health. Avoid sticky or hard foods that could stress the implant, especially during the initial healing phase. Quit smoking, as it can exacerbate diabetes-related complications and hinder recovery. Lastly, stay hydrated—proper hydration supports gum health and reduces the risk of dry mouth, a common issue for diabetics that can lead to bacterial growth.
Trending FAQs on Dental Implants for Diabetics
Here are answers to some frequently asked questions that Whitehouse residents often search for:
- How long does it take for a diabetic to heal after dental implant surgery? Healing typically takes 3-6 months, but it may be slightly longer for diabetics due to slower recovery. Good glucose control can speed this up.
- Are there specific risks for diabetics with dental implants? Yes, risks include delayed healing, infection, and implant failure, particularly if blood sugar is uncontrolled.
- Can I get dental implants if my diabetes is not well-controlled? It’s best to wait until your diabetes is under control, as high glucose levels increase the risk of complications.
- What type of dental implant is best for diabetics? The type depends on your oral health, not diabetes. Your dentist will recommend the best option, often standard titanium implants.
These answers address common concerns, helping you feel more confident about the process.
Finding the Right Dental Implant Provider
Choosing a skilled provider is crucial for a successful outcome. If you’re searching for “dental implants near me“, Whitehouse has several reputable options. Look for a dentist with experience in treating diabetic patients, as they’ll understand the nuances of your care needs. Check for board certification, patient reviews, and a focus on personalized treatment plans. A local expert can guide you through the process, ensuring your implants are placed with precision and care.
Take the Next Step Toward a Confident Smile
Dental implants can be a life-changing solution for diabetics in Whitehouse, offering a path to a fully restored smile. By understanding the process, managing your diabetes, and partnering with a skilled dentist, you can achieve excellent results. Take the first step by scheduling a consultation with a local professional to explore your options and start your journey toward better oral health.

by 110 Dental & Orthodontics | May 16, 2025 | Dental Implants
Dental implant surgery is a transformative procedure that can restore your smile and confidence, offering a permanent solution for missing teeth. If you’ve recently undergone this surgery or are considering it, you’re likely wondering about the recovery process, particularly when it comes to your diet. Eating is a fundamental part of daily life, and understanding how dental implant surgery affects your ability to enjoy meals is crucial for a smooth recovery. In this blog, we’ll explore what you can expect when it comes to eating after dental implant surgery, provide practical tips for managing your diet during recovery, and address common concerns to help you navigate this journey with ease.
Understanding Dental Implant Surgery and Its Impact on Eating
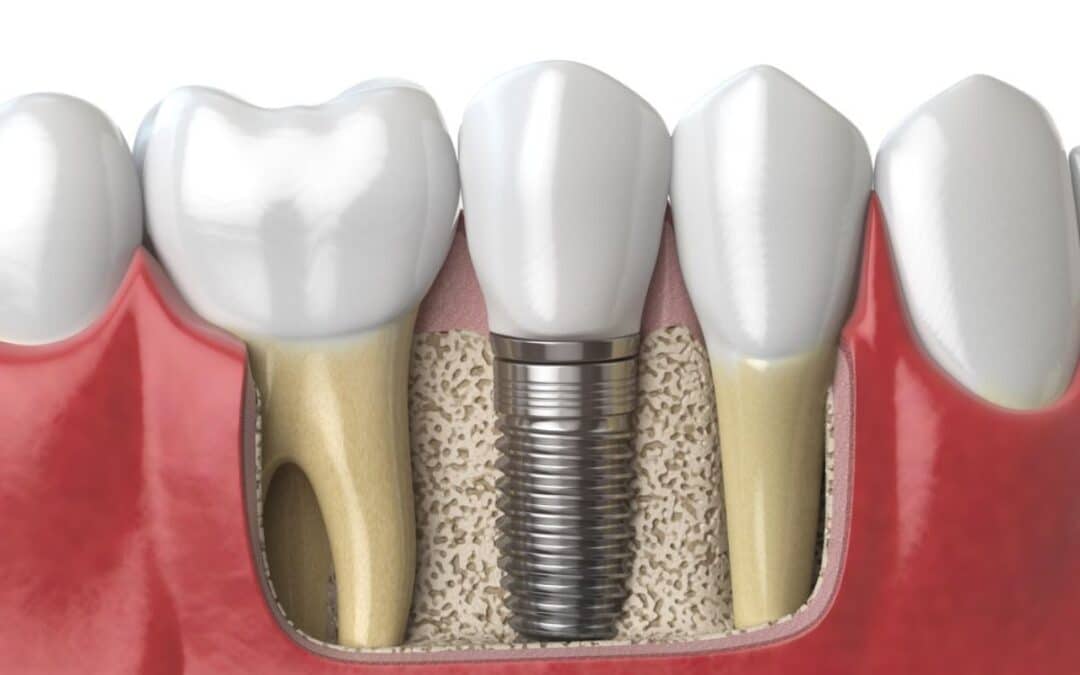
Dental implants are titanium posts surgically inserted into the jawbone to act as artificial tooth roots. These posts fuse with the bone through a process called osseointegration, providing a stable foundation for crowns, bridges, or dentures. While implants are designed to mimic natural teeth in both function and appearance, the surgical process requires a healing period during which your diet needs careful consideration. Immediately after surgery, your gums and jawbone are sensitive, and eating normally right away can disrupt healing or even damage the implant site. The good news? With the right approach, you’ll be back to enjoying your favorite foods in no time.
The First 48 Hours: What to Eat Right After Surgery
The initial 48 hours after dental implant surgery are critical for healing. During this time, your focus should be on minimizing pressure on the surgical site and avoiding irritation. Stick to a soft, liquid, or semi-liquid diet to ensure comfort and promote recovery. Here are some safe options:
- Smoothies (without seeds or hard chunks)
- Broth-based soups (lukewarm, not hot)
- Applesauce or mashed bananas
- Yogurt or pudding
- Protein shakes (blended thoroughly)
Avoid hot foods and drinks, as they can increase swelling or cause discomfort. Also, steer clear of using a straw, as the suction can dislodge the blood clot forming at the surgery site, potentially leading to a painful condition called dry socket. Opt for nutrient-rich foods to support healing—think high-protein options like Greek yogurt or blended lentils, which can aid tissue repair.
Weeks 1 to 2: Transitioning to Soft Foods
As you move into the first and second weeks post-surgery, your mouth will start to feel less tender, but you’re still not ready for a full return to normal eating. At this stage, you can begin incorporating slightly firmer soft foods into your diet while continuing to avoid anything that requires heavy chewing. Some good choices include:
- Mashed potatoes or sweet potatoes
- Scrambled eggs
- Oatmeal or cream of wheat
- Soft-cooked vegetables (like steamed carrots or zucchini)
- Pasta (well-cooked and cut into small pieces)
During this period, it’s still important to avoid hard, crunchy, or sticky foods like nuts, chips, or caramel, as they can irritate the implant site or get lodged in the healing tissues. If you’re in the area and looking for personalized advice, professionals specializing in dental implants in Whitehouse can offer tailored guidance on managing your diet during recovery. Be sure to chew on the opposite side of your mouth from the implant site to minimize pressure and ensure proper healing.
Weeks 3 to 6: Gradually Returning to Normal Eating
By the third to sixth week, most patients notice significant improvement in comfort and can start reintroducing a wider variety of foods. At this point, osseointegration is progressing, and the implant is becoming more stable. You can now experiment with foods that require light chewing, such as:
- Soft breads or tortillas
- Cooked rice or quinoa
- Tender meats (like shredded chicken or fish)
- Soft fruits (like bananas or avocados)
Even as you expand your diet, continue to avoid extremely hard or tough foods, such as raw carrots, apples, or steak, which can place undue stress on the implant. If you’re unsure about your progress, a quick visit to a dentist near Whitehouse, TX, can provide reassurance and ensure your recovery is on track. Additionally, if you’re looking for a specialist to monitor your implant’s long-term success, searching for a “prosthodontist near me” can connect you with experts in restorative dentistry who can offer ongoing support.
Long-Term Eating Habits: Enjoying Food with Dental Implants
Once osseointegration is complete—typically after 3 to 6 months—your dental implant should feel as secure as a natural tooth. At this stage, most patients can eat normally, enjoying a wide range of foods without restrictions. Dental implants are designed to handle the same chewing forces as natural teeth, meaning you can savor crunchy vegetables, chewy breads, and even the occasional hard candy without worry. However, maintaining good oral hygiene is key to ensuring your implant’s longevity. Brush and floss regularly, and schedule routine checkups to keep your implant and surrounding gums healthy.
It’s also worth noting that while implants are highly durable, they’re not indestructible. Avoid habits like chewing on ice or using your teeth to open packaging, as these can damage both implants and natural teeth. By adopting mindful eating habits, you’ll ensure your implant remains a reliable part of your smile for years to come.
Tips for a Smooth Dietary Transition After Surgery
To make your recovery as seamless as possible, here are some practical tips for managing your diet after dental implant surgery:
- Stay Hydrated: Drink plenty of water to keep your mouth clean and support overall healing.
- Eat Nutrient-Dense Foods: Focus on foods rich in vitamins and minerals, like leafy greens (blended into smoothies) or eggs, to aid recovery.
- Cut Food into Small Pieces: Even as you progress to firmer foods, smaller bites are easier to manage and reduce strain on the implant site.
- Avoid Spicy or Acidic Foods: These can irritate the surgical area, especially in the early stages of healing.
- Listen to Your Body: If a particular food causes discomfort, give your mouth more time to heal before trying it again.
By following these guidelines, you’ll support your body’s natural healing process and get back to enjoying meals sooner.
Trending FAQs on Eating After Dental Implant Surgery
To address common concerns, here are answers to some frequently asked questions about eating after dental implant surgery, based on what people often search for on Google:
- How long after dental implant surgery can I eat normally?
Most patients can return to normal eating within 3 to 6 months, once the implant fully integrates with the jawbone, though soft foods are recommended for the first few weeks.
- Can I eat solid food after dental implant surgery?
Solid foods should be avoided for at least the first 1-2 weeks. Gradually reintroduce them after 3-6 weeks, starting with softer options and avoiding hard or crunchy items.
- What foods should I avoid after dental implant surgery?
Steer clear of hard, sticky, or crunchy foods like nuts, popcorn, and caramel, as well as hot or spicy foods that can irritate the surgical site.
- Can I drink coffee after dental implant surgery?
It’s best to avoid hot coffee for the first 48 hours, as it can increase swelling. Opt for lukewarm or cold beverages and avoid using a straw.
These answers aim to clarify common concerns and help you feel more confident about your recovery.
Dental implant surgery is a life-changing procedure that can restore both function and aesthetics to your smile, but it requires patience and care during the recovery process. While you won’t be able to eat normally right away, a gradual approach to reintroducing foods will ensure your implant heals properly and becomes a seamless part of your daily life. By following your dentist’s advice and making mindful dietary choices, you’ll be back to enjoying all your favorite meals in just a few months. If you have concerns or need personalized guidance, don’t hesitate to reach out to a dental professional to support you on this journey.
by 110 Dental & Orthodontics | Apr 17, 2025 | Dental Implants
When the Game Gets Rough: A Real Concern for Teen Smiles
High school sports are more than just extracurricular activities—they’re a passion, a team, a lifestyle. Whether it’s football, basketball, soccer, or hockey, teens give their all. But unfortunately, contact sports often come with risks, including dental injuries. A chipped, broken, or completely knocked-out tooth can affect a teen’s smile, confidence, and even long-term oral health.
That’s where dental implants in Whitehouse come into the picture. More than just a cosmetic fix, dental implants offer a stable, permanent solution for teens who’ve lost teeth due to sports-related trauma.
Why Tooth Replacement Matters for Teens
A missing tooth can do more than affect appearance. It can lead to problems with chewing, speaking, and even shifting of surrounding teeth. Over time, untreated tooth loss may also impact jawbone health, making it essential to find a reliable long-term solution.
For teens whose facial bones have finished developing—typically around age 17 or older—dental implants are often considered a safe and highly effective replacement option.
What Makes Dental Implants Ideal for Teen Athletes?
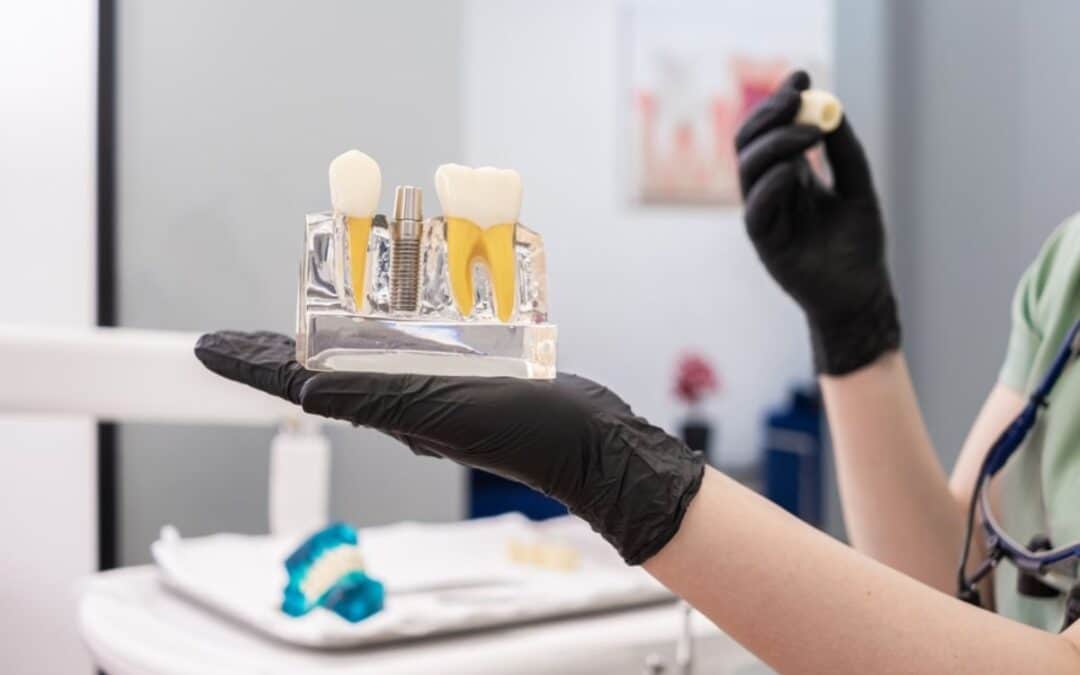
Unlike dentures or bridges, dental implants replace both the tooth and its root, which means they offer unmatched stability and function. They’re durable, natural-looking, and designed to last for decades with proper care.
Here’s why dental implants are an especially great choice for active teens:
1. Restores Confidence
Losing a tooth at a young age can be emotionally challenging. Dental implants look and feel just like natural teeth, helping teens regain their confidence on and off the field.
2. Preserves Oral Health
Implants prevent bone loss and support neighboring teeth. This helps maintain the natural shape of the jaw and prevents the shifting that often occurs with missing teeth.
3. Built for an Active Lifestyle
Teen athletes are constantly on the go, and implants require no special maintenance beyond normal brushing and flossing. There’s no need to worry about them slipping or getting in the way during sports or social activities.
4. Long-Term Stability
Because dental implants are fused to the jawbone, they provide lasting support. Unlike temporary solutions, implants won’t need to be replaced or adjusted frequently—ideal for a busy teen’s life.
When Are Teens Eligible for Dental Implants?
Not every teen is ready for implants immediately after an injury. A professional evaluation is essential to determine jaw development and oral health status. If a teen’s jaw is still growing, temporary solutions may be recommended until implant placement becomes viable.
After bone maturity is confirmed, the implant process involves careful planning, minor surgery, and follow-up care. The result is a permanent, fully functional tooth that blends seamlessly into the smile.
The Role of Preventive Care and Mouthguards
While dental implants offer a strong solution after an injury, prevention is always better. A custom-fitted mouthguard can protect teeth during sports and significantly reduce the risk of dental trauma. Encourage your teen to wear one during practices and games—it’s a simple step that can save their smile.
Sports injuries are a common part of teen life, but losing a tooth doesn’t have to mean losing confidence. With modern dentistry, teens have access to long-lasting solutions that restore both function and appearance. Dental implants in Whitehouse offer a durable and natural-looking way to recover from dental trauma—and keep smiling with pride.
For compassionate guidance and expert care, consult a trusted dentist in Whitehouse, OK, who understands your teen’s needs and lifestyle.
by 110 Dental & Orthodontics | Apr 3, 2025 | Dental Implants
Dental implants are a long-term solution for replacing missing teeth, offering durability, functionality, and a natural appearance. However, just like natural teeth, implants require proper care to stay healthy. One potential issue that patients might face is an infection around the implant, also known as peri-implantitis. If left untreated, this condition can compromise the stability of the implant and even lead to implant failure. In this blog, we’ll explore whether a dental implant can get infected, the warning signs to watch for, and the best solutions for keeping your implant healthy.
Can a Dental Implant Really Get Infected?
Yes, dental implants can become infected, but it’s important to understand why. While the implant itself is made of titanium and cannot decay like natural teeth, the surrounding gum and bone tissue are still vulnerable to bacteria. Infection can occur if bacteria accumulate around the implant, leading to inflammation and potential damage to the supporting structures.
Common Causes of Dental Implant Infections:
- Poor oral hygiene leading to plaque buildup around the implant
- Smoking, which reduces blood flow and slows healing
- Pre-existing gum disease that weakens the gums and bone
- Uncontrolled diabetes or other conditions that affect healing
- Excessive force on the implant due to teeth grinding or misalignment
If you have dental implants in Whitehouse, it’s crucial to follow a good oral hygiene routine and attend regular dental checkups to prevent infection.
Warning Signs of an Infected Dental Implant
Recognizing the early signs of infection can help you seek timely treatment and prevent serious complications. Here are some symptoms to watch for:
1. Redness and Swelling
Mild swelling after implant placement is normal, but persistent or worsening swelling around the implant site may indicate an infection.
2. Bleeding Gums (Peri-Implant Mucositis)
If your gums bleed when you brush or floss around the implant, it could be an early sign of infection. Healthy gums should not bleed easily.
3. Pain or Discomfort
Some discomfort is normal after surgery, but sharp or persistent pain long after the healing process may be a warning sign of infection.
4. Pus or Bad Taste in the Mouth
If you notice pus, a foul taste, or bad breath that won’t go away, it may indicate a bacterial infection around the implant.
5. Loose Implant or Difficulty Chewing
A healthy implant should feel stable, just like a natural tooth. If you experience movement or discomfort when chewing, it could be a sign of bone loss due to infection.
Solutions for Treating an Infected Dental Implant
The good news is that if caught early, an infected dental implant can often be treated successfully. The right treatment will depend on the severity of the infection:
1. Professional Cleaning and Antibiotics
For mild infections, a deep cleaning around the implant and a round of antibiotics may be enough to eliminate bacteria and restore gum health.
2. Laser Therapy or Antibacterial Rinse
Some dentists use laser therapy or specialized mouth rinses to target bacteria and promote healing around the implant.
3. Surgical Intervention (If Necessary)
In more advanced cases, surgical treatment may be needed to remove infected tissue and regenerate lost bone around the implant.
4. Implant Replacement (Severe Cases)
If the infection has caused significant bone loss and the implant is no longer stable, it may need to be removed and replaced after a healing period.
How to Prevent Implant Infections
Taking preventive measures is the best way to avoid infection and ensure the long-term success of your implant. Here are some key tips:
- Brush and floss daily to remove plaque buildup around the implant.
- Use an antibacterial mouthwash to help control bacteria in the mouth.
- Avoid smoking as it weakens the gums and slows healing.
- Visit your dentist regularly for professional cleanings and checkups.
- Be mindful of what you eat, avoiding overly hard or sticky foods that may stress the implant.
While dental implants are a reliable and effective solution for tooth loss, they require proper care to stay healthy. Infection can occur, but by recognizing the warning signs early and seeking professional treatment, you can prevent complications and ensure long-term success. If you’re experiencing any symptoms of infection or have concerns about your dental implants, reach out to a dentist near you for expert care and guidance.

by 110 Dental & Orthodontics | Jan 28, 2025 | Dental Implants
Dental implants are one of the most effective ways to restore missing teeth, offering durability, functionality, and a natural appearance. However, if you’re considering dental implants in Whitehouse, you may have questions about their potential impact on your sinuses—especially if you’re getting implants in the upper jaw.
While dental implants are generally safe and successful, improper placement or pre-existing conditions can sometimes lead to sinus complications. Let’s explore how dental implants and sinuses are connected, potential risks, and how to ensure a smooth, problem-free procedure.
Understanding the Connection Between Dental Implants and Sinuses
Your maxillary sinuses are air-filled cavities located just above the upper jaw. When teeth in the upper jaw are lost, the bone underneath naturally shrinks due to a lack of stimulation. In some cases, this leaves very little bone to support an implant.
If an implant is placed without enough bone support, it may extend too far into the sinus cavity, potentially causing discomfort, infection, or sinus-related complications. This is why skilled dentists conduct detailed evaluations before recommending dental implants in Whitehouse, ensuring there is sufficient bone density to support the implant. If necessary, a sinus lift procedure can be performed to add bone and create a stable foundation.
Potential Sinus Problems Caused by Dental Implants
While dental implants have a high success rate, there are cases where they can contribute to sinus issues. Here are four potential complications:
1. Sinus Perforation
If an implant is placed too deep, it may puncture the sinus membrane. This can lead to nasal congestion, discomfort, or even chronic sinusitis. In severe cases, surgery may be required to repair the sinus and reposition the implant.
2. Sinus Infections (Sinusitis)
When the sinus lining is disturbed by an improperly placed implant, bacteria may enter, leading to an infection. Symptoms may include headaches, facial pain, post-nasal drip, and nasal congestion. If left untreated, a sinus infection can spread and become more serious.
3. Implant Failure Due to Poor Bone Support
If an implant doesn’t integrate properly with the surrounding bone due to its proximity to the sinus cavity, it may become loose or even fail. This can lead to discomfort and the need for removal or replacement.
4. Persistent Sinus Pressure or Discomfort
Even if an implant does not perforate the sinus, it can still press against it, causing a sensation of pressure or mild discomfort. This issue often resolves as healing progresses, but in some cases, adjustments may be needed.
Preventing Sinus Problems from Dental Implants
While sinus-related issues are uncommon, proper planning can help prevent them. Here are five key steps to minimize risks:
1. Comprehensive Pre-Implant Evaluation
A skilled dentist will use advanced imaging, such as CBCT (cone beam computed tomography) scans, to assess the position of your sinuses, bone density, and implant placement.
2. Sinus Lift Surgery if Necessary
If your upper jawbone is too thin, a sinus lift can help create a solid foundation by adding bone to the area, ensuring implants do not interfere with the sinuses.
3. Choosing an Experienced Implant Specialist
Proper implant placement is key to avoiding sinus complications. Choosing a highly trained and experienced dental professional can significantly reduce risks.
4. Following Post-Surgery Care Instructions
Patients should follow post-operative care guidelines, including avoiding excessive sneezing or nose-blowing, which could put pressure on the sinus area.
5. Monitoring for Early Symptoms
If you experience persistent sinus pressure, nasal congestion, or pain after your procedure, consult your dentist promptly. Early intervention can prevent complications from worsening.
What to Do If You Experience Sinus Problems After a Dental Implant?
If you suspect that a dental implant is causing sinus issues, here’s what you should do:
- Consult your dentist immediately. They will examine the area and take X-rays or a CT scan to determine if the implant is affecting your sinuses.
- Take prescribed medications. If an infection is present, antibiotics or anti-inflammatory medication may be recommended.
- Consider implant repositioning. In severe cases, the implant may need to be adjusted or removed to relieve sinus pressure.
- Undergo sinus repair surgery. If the sinus membrane has been perforated, a specialist may perform a minor surgical procedure to correct the issue.
Are Dental Implants Still a Safe Choice for Upper Jaw Replacements?
Yes! Despite the potential for sinus complications, dental implants remain a highly effective and safe solution for replacing missing teeth in the upper jaw. With proper evaluation, planning, and expert placement, most patients experience successful outcomes without sinus-related issues. Advances in technology, such as 3D imaging and guided implant surgery, have further improved accuracy and safety.
If you’re considering dental implants but have concerns about your sinuses, speaking with a dentist near you can provide clarity and reassurance. A professional assessment will determine if implants are the right solution for you and ensure a smooth, comfortable process.








