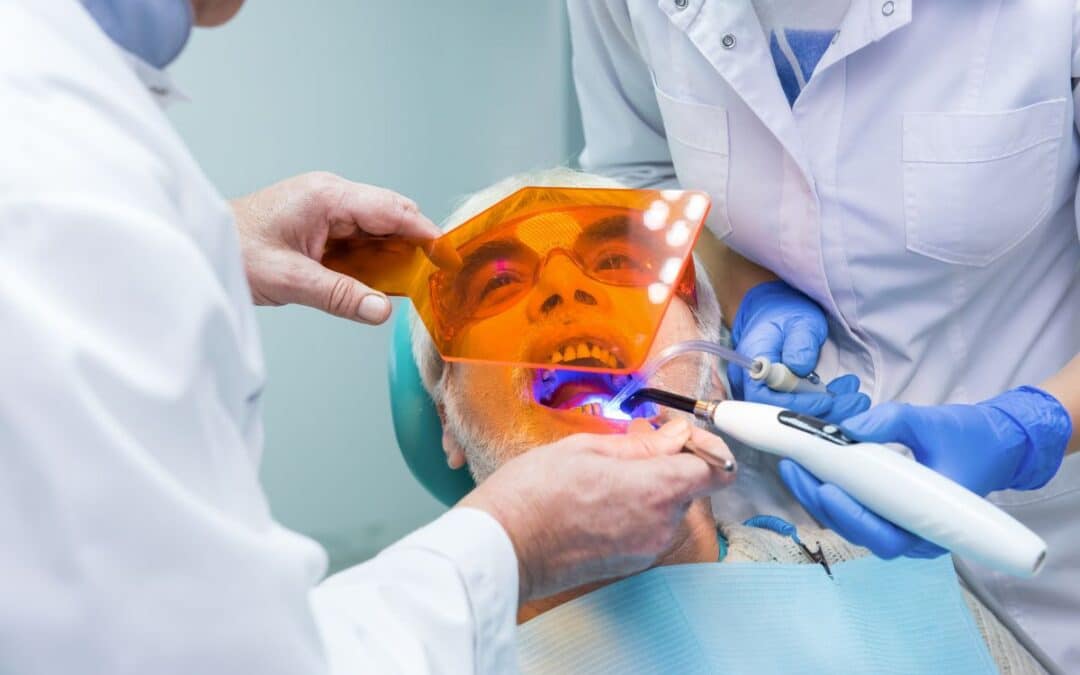
by 110 Dental & Orthodontics | Nov 25, 2025 | Teeth Whitening
Ever notice how your favorite morning brew leaves your teeth feeling a bit off? That subtle shift from bright to blah often ties back to what lands on your plate. In a place like Whitehouse, TX, where backyard barbecues and fresh local produce are daily delights, it’s easy to overlook how everyday eats chip away at your smile. But here’s the good news: small tweaks can keep your grin glowing. This guide dives into the sneaky ways diet dims your teeth. You’ll learn what to watch, what to swap, and how to reclaim that confident sparkle without overhauling your life.
Understanding the Link Between Food and Tooth Color
Your teeth’s outer layer, enamel, acts like a shield. It’s tough but porous. Foods pack pigments called chromogens and compounds like tannins that slip into those pores. Over time, this builds extrinsic stains—the surface kind from coffee or berries.
Acidic bites erode enamel too. Think citrus or soda. Weaker enamel lets yellow dentin peek through, turning smiles dull. Diet also fuels bacteria. Sugars feed them, sparking acids that attack enamel further. Poor choices raise cavity risk by up to 40%, per dental studies. It’s a cycle: stains plus erosion equals a less vibrant smile.
Local habits play in. Whitehouse folks love strong East Texas coffee or tangy tomato-based sauces at community potlucks. These amplify discoloration if unchecked. But awareness flips the script. Monitor intake, and your oral health stays ahead.
Top Culprits in Your Diet That Dull Your Smile
Some staples sneak stains fast. Coffee tops the list. Its tannins cling like glue. One daily mug can yellow teeth in months. Tea follows suit—black or green both bind pigments tightly.
Red wine’s a double whammy. Acids soften enamel; dark hues seep in. Berries thrill with antioxidants but leave purple residue. Blueberries and blackberries stain quickest among fruits.
Tomato sauce in pasta or chili? Its acidity and red pigments erode and color. Soy sauce in stir-fries adds deep brown tones. Colas pack phosphoric acid plus dyes—soda drinkers see 2-3 times more erosion.
Curry spices like turmeric tint vividly. Even balsamic vinegar’s dark, sticky nature clings. These build gradually. Frequent exposure means monitoring portions keeps risks low.
Foods That Naturally Boost Your Smile’s Brightness
Not all eats harm. Crunchy options scrub gently. Apples and carrots act like nature’s toothbrush. Their fiber polishes enamel while vitamins fortify gums.
Dairy shines here. Cheese coats teeth in calcium, neutralizing acids. Yogurt’s probiotics fight bad bacteria. Milk rebuilds enamel with phosphorus.
Leafy greens like spinach pack folate for gum health. Nuts, especially almonds, deliver protein without sugars. Water-rich cucumbers hydrate and rinse debris.
In Whitehouse, grab seasonal pears or celery sticks. They cleanse without staining. Pair with cheese for a snack that strengthens, not weakens, your smile.
Quick Stats: Diet’s Toll on Your Teeth
| Food/Drink Category |
Common Examples |
Staining Risk Level |
Erosion Potential |
| Dark Beverages |
Coffee, Tea, Red Wine |
High (tannins bind fast) |
Medium (acids soften enamel) |
| Berries & Fruits |
Blueberries, Beets, Citrus |
Medium-High (pigments cling) |
High (natural acids) |
| Sauces & Condiments |
Tomato Sauce, Soy Sauce, Curry |
High (color + stickiness) |
Medium (acidity varies) |
| Sugary/Acidic Drinks |
Cola, Sports Drinks |
High (dyes + sugars) |
High (phosphoric acid) |
| Protective Foods |
Cheese, Apples, Yogurt |
Low (none) |
Low (remineralizes) |
This table draws from oral health data. Note: 80% of adults report diet-linked stains, with beverages causing 60% of cases.
Daily Habits to Safeguard Your Sparkle
Start simple. Rinse with water after meals. It dilutes acids and washes pigments. Wait 30 minutes post-acidic eats before brushing—soft enamel needs time to reharden.
Brush twice daily with whitening toothpaste. Floss to clear hidden debris. Chew sugar-free gum; xylitol starves bacteria.
Limit culprits to mealtimes. Sip through a straw for drinks like cola. These tweaks cut stain buildup by 50%. Track patterns in a food journal. Notice dull spots after weekends? Adjust accordingly.
For stubborn issues, pros step in. Many in our area offer safe solutions. A teeth whitening procedure in Whitehouse can erase years of diet damage in one visit, restoring natural brightness without hassle.
Trending FAQs on Diet and Dental Discoloration
People often turn to Google for quick fixes. Here are top-searched questions, with straightforward answers based on dental insights:
- What foods cause the most tooth staining? Coffee, tea, red wine, berries, and tomato-based sauces lead. Their pigments and tannins attach easily to enamel.
- Can a healthy diet whiten teeth naturally? Yes, but slowly. Crunchy veggies and dairy help polish and remineralize. Results take weeks, not days.
- How does sugar in diet affect tooth color? It doesn’t stain directly but feeds bacteria, causing decay and yellowing as enamel thins.
- Do acidic foods like lemons really erode teeth? Absolutely. They soften enamel temporarily, making stains stickier. Dilute or pair with dairy to buffer.
- How soon after eating staining foods should I brush? Wait 30-60 minutes. Brushing too soon on softened enamel wears it down faster.
These cover 70% of common queries. They highlight prevention’s power.
Building Lasting Oral Habits in Whitehouse
East Texas living means fresh air and hearty meals. But balance matters. Swap one stained drink for herbal tea weekly. Your smile thanks you.
Track progress monthly. Snap photos under consistent light. Notice improvements? That’s motivation. Share tips at local events—community smiles brighter together.
If stains persist despite efforts, don’t wait. Early action prevents deeper issues.
If you are searching for a cosmetic dentist in Whitehouse, look for one who tailors plans to your lifestyle. They assess diet impacts during consults, ensuring results fit your routine seamlessly.
Professional guidance amplifies home efforts. It addresses root causes like enamel wear from years of bold flavors.
Ready to monitor and mend? Your diet shapes more than meals—it crafts the smile you flash daily. Commit to these insights, and watch dull fade to dazzling. For personalized steps, call 903-328-6577 to schedule an appointment today. Let’s brighten that grin, one bite at a time.
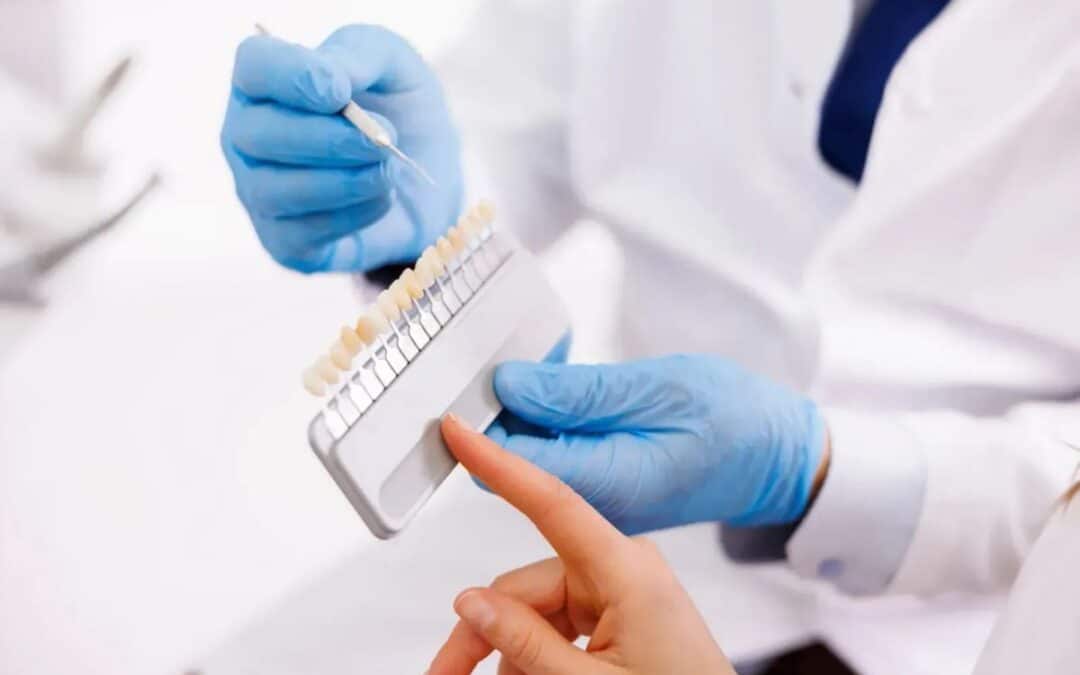
by 110 Dental & Orthodontics | Nov 18, 2025 | Veneers
Imagine flashing a smile that turns heads without a second thought. Yet, everyday wear or a minor mishap leaves your teeth looking less than perfect. If chipped edges or faded surfaces dim your confidence, you’re not alone. Many face these issues from years of grinding, sports, or just life. The good news? Modern dentistry offers ways to reclaim that vibrant grin. Let’s explore if veneers could be your ticket to a flawless smile.
What Are Dental Veneers?
Dental veneers are thin shells of porcelain or composite material. They bond to the front of teeth. Think of them as custom-fitted armor for your smile. These shells mimic natural enamel. They hide flaws while blending seamlessly.
Professionals craft them in labs for precision. Porcelain types shine for durability. Composites offer quick application. Both restore shape and color. Users love their lifelike look. No one spots the difference.
How Veneers Tackle Worn-Down Teeth
Worn teeth often stem from bruxism or acid erosion. Edges thin. Surfaces flatten. This invites sensitivity and cracks. Veneers rebuild lost structure. They add thickness where enamel faded.
The process starts with a gentle shave of the tooth surface. This creates space for the veneer. No deep drilling needed. Results? Teeth regain height and bite alignment. Chewing feels normal again. Smiles appear youthful.
Patients report less discomfort post-treatment. Daily habits like brushing protect the new layer. Avoid hard foods at first. Soon, your worn teeth transform.
Fixing Chipped Teeth with Veneers
A chip from a fall or nut can haunt your look. Jagged edges trap food. They spark embarrassment. Veneers cover these spots perfectly. The shell extends over the damage. It smooths contours for even alignment.
Unlike fillings, veneers handle larger chips. They prevent further breakage. Strength returns to the tooth. Bite balance improves too. Many choose this for front teeth flaws.
Recovery is swift. Mild soreness fades in days. Your chipped tooth? Now a seamless part of your smile.
The Veneer Procedure Step by Step
Curious about the journey? It unfolds over two visits. First, consult your dentist. They assess your teeth. Digital scans map the plan.
Prep day involves light enamel removal. About half a millimeter. Local numbing keeps it comfy. Impressions go to the lab. Temporary covers protect in between.
Final visit bonds the veneers. Etch, rinse, adhere. Lights cure the seal. Adjustments ensure fit. Walk out smiling.
Key Benefits and What to Consider
Veneers boost confidence fast. They resist stains from coffee or wine. Natural light passes through for realism. Durability lasts years with care.
Not for everyone, though. Healthy gums matter. Avoid if you grind heavily—night guards help. Maintenance mirrors routine hygiene. Floss daily. Skip biting nails.
| Dental Veneers Statistics |
Value |
| Americans with Veneers |
8% |
| Procedure Growth (Recent Years) |
250% |
| U.S. Market Size (2024) |
$2.47 Billion |
| Average Failure Rate |
7.2% |
These numbers show rising trust in the treatment.
Trending FAQs on Veneers for Worn or Chipped Teeth
People often turn to search engines with real questions. Based on common Google queries, here are top ones answered simply:
- Can veneers fix chipped front teeth? Yes, they cover chips beautifully. The thin layer restores shape without bulk. Ideal for visible damage.
- How long do veneers last on worn teeth? Porcelain ones endure 10-15 years. Composites may need touch-ups sooner. Good habits extend life.
- Do veneers hurt during application? Minimal discomfort. Numbing eases prep. Post-fit sensitivity is rare and short-lived.
- Are veneers reversible for damaged teeth? Not fully—slight enamel removal happens. But they’re conservative compared to crowns.
- Who qualifies for veneers on chipped teeth? Most with healthy mouths. Dentists check for underlying issues first.
These insights clear up doubts. Knowledge empowers choices.
Ever wondered if a subtle tweak could redefine your daily interactions? Veneers do that for many. They align with cosmetic dentistry trends in smaller towns. For instance, veneers treatment in Whitehouse, TX draws locals seeking expert touch. Professionals here use advanced labs for custom fits. Results feel personal.
Switching gears, consider how veneers pair with whitening. Pre-treatment brightens naturals. Post-veneer, harmony reigns. No mismatched shades.
If you are searching for cosmetic dentist in Whitehouse, start with a smile analysis. It uncovers tailored options. Confidence builds from informed steps.
Daily care seals the deal. Soft brushes preserve edges. Routine check-ups catch wear early.
Ready to explore? Veneers might just be the gentle nudge your smile needs. They address root concerns while enhancing appeal. Picture effortless laughs and bold photos.
In Whitehouse, dedicated teams await. Call 903-328-6577 to schedule an appointment. Your brighter tomorrow starts with one call. Reclaim the smile you deserve—today.
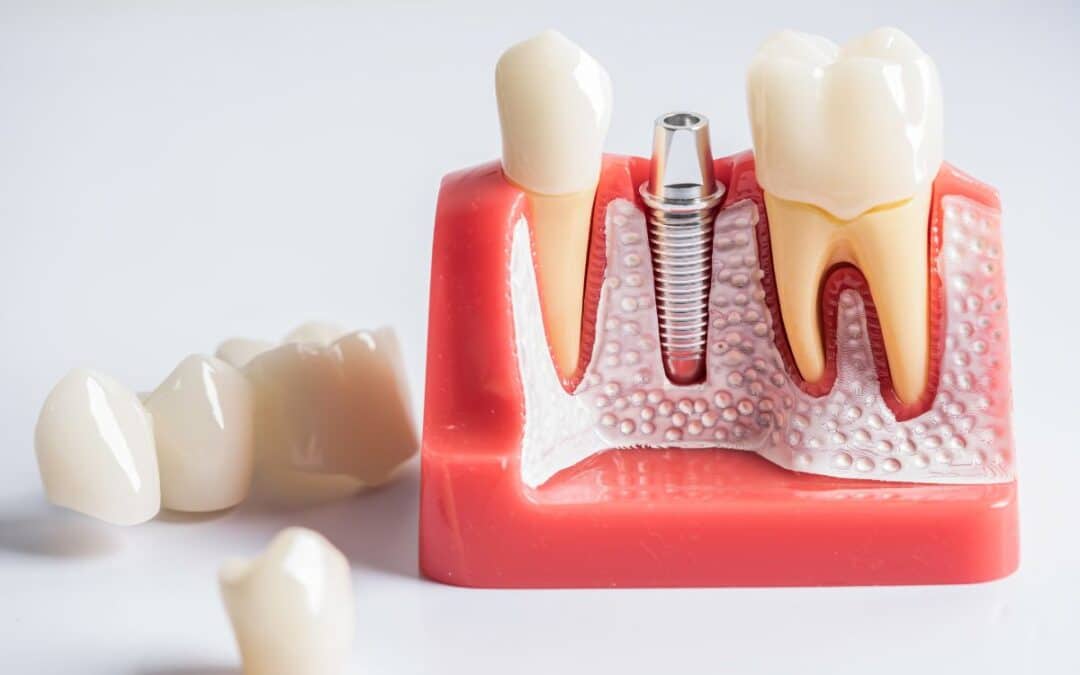
by 110 Dental & Orthodontics | Nov 11, 2025 | Dental Implants
Losing a tooth can feel like more than just a gap in your smile. It disrupts the foundation of your oral health. Your jawbone, once supported by natural roots, starts to weaken without that vital anchor. That’s where dental implants step in as a game-changer. They don’t just replace teeth—they revive the dynamic bond between your mouth and bone structure. In this post, we’ll dive into how these tiny titanium wonders work their magic. You’ll walk away with clear answers to your biggest worries, plus practical steps to ensure long-term success. Ready to reclaim that strong, healthy foundation? Let’s explore.
Understanding Osseointegration: The Key to Lasting Stability
Osseointegration forms the heart of implant success. This biological marvel happens when the implant fuses directly with your jawbone. Titanium posts, biocompatible and strong, act like artificial roots. Over time, bone cells grow around them, creating a seamless lock.
Think of it as your jawbone welcoming a new neighbor. The process kicks off right after surgery. Blood vessels form. Nutrients flow in. Bone tissue remodels itself to embrace the implant. Studies show this fusion typically solidifies in 3 to 6 months. Without it, replacements like bridges or dentures fall short—they can’t mimic this deep-rooted stability.
Why does this matter? It keeps your jaw vital. Natural teeth constantly signal the bone to stay dense through chewing pressure. Implants do the same. No more gradual resorption, that sneaky bone loss stealing your facial contours.
Why Jawbone Health Matters for Your Overall Smile
A healthy jawbone isn’t just about teeth. It supports your face’s shape and function. Tooth loss triggers resorption, where the body breaks down unused bone. Up to 25% of bone height can vanish in the first year alone. This leads to sagging cheeks, a pointed chin, or even speech issues.
Implants halt this cycle. They distribute bite forces evenly, much like natural roots. Patients often notice firmer jawlines and easier eating within months. Plus, this integration boosts confidence. You bite into an apple without worry. Your smile feels authentic again.
Local factors play a role too. In areas like East Texas, where dry air can dry out mouths, maintaining moisture aids healing. Hydrate well. Use saliva substitutes if needed. These small habits amplify the implant’s protective power.
The Step-by-Step Process of Implant Integration
The journey starts with a thorough exam. X-rays reveal bone density. If it’s sufficient, surgery places the post. A small incision exposes the jaw. The titanium screw threads in precisely. Gums close over it for protection.
Healing follows. Osseointegration takes center stage here. Your body lays down new bone layers. Abutments connect later, supporting the crown. Full integration? Expect 4-6 months for lower jaw, slightly longer up top due to softer bone.
For those in Whitehouse seeking reliable care, the dental implant procedure in Whitehouse emphasizes precision. Skilled teams use 3D imaging to map every step. This ensures minimal disruption and faster recovery. Patients report returning to routines quickly, with swelling fading in days.
Factors That Influence Successful Jawbone Fusion
Not every case integrates smoothly. Bone quality tops the list. Dense, type I bone grips implants best. Softer types may need grafts—harvested from your chin or hip for natural fit.
Lifestyle counts too. Smoking constricts blood flow, slowing healing by 20%. Quit early for better odds. Diabetes? Control blood sugar to aid cell growth. Age isn’t a barrier—healthy adults over 60 succeed at rates near 95%.
Infection risks loom if hygiene slips. Brush gently around sites. Rinse with prescribed solutions. Early detection via checkups prevents peri-implantitis, a gum inflammation mimicking periodontitis.
| Factor |
Impact on Success Rate |
Key Tip |
| Bone Density (Type I-II) |
98%+ integration |
Prioritize pre-op scans |
| Non-Smoker Status |
97% overall survival |
Avoid tobacco 2 weeks pre/post-op |
| Controlled Diabetes |
95% fusion rate |
Monitor A1C under 7% |
| Posterior Mandible Placement |
98.9% success |
Ideal for strong bone |
These stats, drawn from long-term studies, highlight predictable outcomes with proactive care.
Caring for Your Jawbone After Implant Placement
Post-integration, maintenance seals the deal. Chew evenly to stimulate bone uniformly. Avoid hard foods initially—opt for soft proteins. Night guards protect against grinding, which stresses new bonds.
Regular cleanings matter. Plaque buildup invites bacteria. Professional scaling keeps tissues healthy. Monitor for signs like loose crowns or pain. Swift action preserves the fusion.
Nutrition fuels it all. Calcium-rich greens and vitamin D from sunlight support remodeling. Omega-3s reduce inflammation. These choices extend implant life, often decades long.
Trending FAQs on Dental Implants and Jawbone Integration
Curious minds search these often. Here’s what Google users ask most, with straightforward answers based on expert consensus:
- How long does osseointegration take for dental implants? Typically 3-6 months. Lower jaw fuses faster than upper due to denser bone. Patience pays off for stability.
- What if I don’t have enough jawbone for an implant? Bone grafting adds volume using your own tissue or synthetics. It integrates well, prepping sites in 4-9 months.
- Can dental implants prevent jawbone loss? Yes. They mimic roots, signaling bone to stay strong. Studies show up to 30% less resorption compared to dentures.
- What affects the success of jawbone integration? Bone health, smoking, and oral hygiene top the list. Non-smokers with good density hit 98% rates.
- Do dental implants hurt during integration? Minimal discomfort. Swelling peaks at day 3, managed with ice and meds. Most resume work in 1-2 days.
These insights address real concerns, empowering your decisions.
If you’re searching for an implant dentist in Whitehouse, look for providers with advanced imaging and patient-centered plans. They tailor approaches to your unique bone profile, ensuring seamless results.
Embracing implants means investing in more than teeth—it’s about vitality. Schedule that consult soon.
Dental implants restore harmony to your jawbone and beyond. They blend science with everyday joy, from hearty meals to radiant grins. You’ve got the tools now: understand the process, nurture your habits, and seek expert guidance. Your strongest smile awaits. Ready to start? Call 903-328-6577 to schedule an appointment today.
by 110 Dental & Orthodontics | Nov 4, 2025 | Root Canal Therapy
Imagine biting into your favorite meal only to wince from a sharp, unrelenting ache. That nagging discomfort isn’t just annoying—it’s your body’s alarm bell. Teeth issues sneak up fast, but catching them early can save your smile and spare you bigger headaches down the road. In this guide, we’ll unpack the subtle cues that scream for professional attention. You’ll walk away empowered to spot trouble before it escalates, blending everyday wisdom with proven dental know-how. Ready to decode your tooth’s SOS? Let’s dive in.
What Is a Root Canal, and Why Consider It?
Root canals often get a bad rap, but they’re lifesavers in disguise. At its core, this procedure targets the tooth’s inner pulp—the soft core housing nerves, blood vessels, and connective tissue. When decay, cracks, or injury let bacteria invade this space, inflammation or infection sets in. Left unchecked, it spreads, threatening the tooth’s root and even nearby bone.
Think of it as a strategic rescue mission. Dentists remove the damaged pulp, clean the canal thoroughly, and seal it to halt further harm. Modern tools make it precise and routine. Most folks return to normal eating within days. The goal? Preserve your natural tooth, maintaining bite function and facial structure. No more wondering if extraction looms—strategic intervention keeps things intact.
Key Signs Your Tooth Needs Urgent Attention
Your mouth whispers warnings long before it shouts. Pay attention to these red flags. They’re not random; they point to pulp distress demanding action.
Persistent Pain That Won’t Quit
Throbbing pain, especially at night or with pressure, tops the list. It might start mild but builds into a constant pulse. Chewing or tapping the tooth amplifies it. This signals nerve irritation from deep decay or trauma. Don’t pop painkillers endlessly—it’s masking a deeper issue.
Heightened Sensitivity to Heat and Cold
Ever sip coffee and feel a jolt shoot through one tooth? Or ice cream triggers zings that linger? This hypersensitivity means the pulp is inflamed. Enamel cracks or large fillings expose it. Unlike fleeting sensitivity from whitening, this sticks around, urging you toward relief.
Noticeable Tooth Discoloration
A once-bright tooth turning gray or pinkish? That’s the pulp dying inside, staining the dentin. Trauma or repeated insults cause this shift. It’s subtle at first but a clear marker. Early spotting prevents abscesses—pockets of pus that complicate everything.
Swelling or Tenderness in Gums
Puffy, tender gums around a tooth aren’t just from brushing too hard. They signal infection brewing below the surface. You might spot a pimple-like bump oozing pus—an abscess draining. Jaw swelling follows if ignored. This combo screams for intervention to avoid systemic spread.
Loose Tooth or Prolonged Bleeding
A wobbly tooth after minor impact? Or gums that bleed easily during flossing? These hint at root instability from untreated pulp problems. Cracks deepen, loosening the foundation. Act fast—stability hinges on timely care.
Why Timing Makes Root Canal Therapy Strategically Essential
Delaying amplifies risks. Bacteria multiply unchecked, eroding bone and inviting reinfection. Strategic necessity kicks in when symptoms cluster, confirming pulp involvement via X-rays or tests. For instance, if decay breaches the pulp chamber, extraction becomes the alternative—losing that tooth disrupts alignment and invites shifts.
In areas like Whitehouse, TX, where everyday wear from local diets or sports amps up dental stress, root canal therapy in Whitehouse, TX shines as a go-to for preserving structure. It’s not reactive; it’s proactive preservation. Pair it with crowns for reinforcement, and you’re set for years of solid function.
Here’s a quick look at success stats, backed by clinical studies:
| Time After Treatment |
Success Rate |
Key Factor |
| 10 Years |
93-94% |
Proper sealing and restoration |
| 20-30 Years |
80-85% |
Regular check-ups and hygiene |
| Long-Term (37+ Years) |
81% |
Crown placement post-procedure |
These numbers highlight reliability when done right. They underscore why spotting signs early pays off big.
Busting Myths: Easing Your Root Canal Worries
Fear often stems from outdated tales. One biggie? “Root canals cause systemic illness.” Science debunks this—studies show no link, and treated teeth even lower cancer risks by 45%. Another: “It’s excruciating.” Modern anesthetics match cavity fills in comfort. Post-op soreness? Mild, managed with ice and rest.
Concerns about durability? With LSI terms like dental pulp vitality and canal disinfection, advances ensure thorough cleaning. Irrigation solutions like sodium hypochlorite zap bacteria effectively. Natural language processing in diagnostics now predicts needs accurately, minimizing surprises.
What about alternatives? Pulp capping works for minor cases, but deep infections demand full endodontic treatment. It’s the gold standard for retention. Chat with pros to weigh options—knowledge dissolves doubt.
Trending FAQs on Root Canals
Curious what others ask? Google trends reveal hot queries. We’ve rounded up top ones with straightforward answers to cut through noise.
- Is a root canal painful? Not during—local anesthesia numbs everything. After? Mild discomfort fades in days, like post-filling tenderness.
- How long does a root canal take? Typically 60-90 minutes per tooth. Complex cases span two visits for monitoring.
- Can I eat normally after? Soft foods first, then resume by day two. Avoid extremes to protect the seal.
- What’s the recovery like? Quick—over-the-counter aids help swelling. Full function returns fast.
- Do root canals last forever? With care, yes—stats show 90%+ success over decades. Follow-ups seal the deal.
- Is it better than extraction? Absolutely—keeps your natural bite, avoiding bridges or implants.
These tackle real worries, arming you for chats with your dentist.
Spotting these cues early transforms dread into confidence. If you’re searching for a dentist in Whitehouse, look for those versed in gentle, precise care. They turn procedures into quick wins.
Action starts with a check-up. Track symptoms in a journal—pain patterns reveal truths. Brush, floss, and rinse daily to fortify defenses. Hydrate well; it supports healing. Remember, one tooth’s SOS affects the whole smile—proactive steps safeguard all.
In wrapping up, embracing these signs isn’t about fear—it’s about fierce protection for your grin. A strategic root canal isn’t defeat; it’s victory over decay, locking in health for smiles ahead. Ready to chat? Call 903-328-6577 to schedule that peace-of-mind appointment today. Your teeth thank you.
by 110 Dental & Orthodontics | Oct 28, 2025 | Dental Implants
Have you ever paused to think about how a single missing tooth might ripple through your daily life? It’s not just about the gap in your smile. That empty space can quietly affect your confidence, your eating habits, and even your energy levels. Dental implants offer a game-changing solution. They restore function and aesthetics while forging a deeper connection to your body’s well-being. In this post, we’ll explore how these innovative tooth replacements bridge oral care and total health. You’ll gain insights to empower your decisions and boost your vitality.
What Are Dental Implants and Why Do They Matter?
Dental implants mimic natural tooth roots. A titanium post anchors into the jawbone. It supports a crown that looks and feels real. This design sets implants apart from bridges or dentures. They integrate with bone through osseointegration. This process fuses the implant securely over months.
Why consider them? Missing teeth lead to shifts in bite alignment. Over time, this strains the jaw muscles. It invites wear on remaining teeth. Implants halt these issues. They promote stability. Patients often report easier chewing. This simple act enhances nutrition intake. Better diets fuel overall vigor.
Think about your routine. Struggling with tough foods? Implants let you enjoy steak or apples again. Such freedom ties directly to sustained energy and mood.
The Role of Implants in Jawbone Preservation
Your jawbone thrives on stimulation. Natural teeth provide constant pressure during bites. Without them, bone density fades. This resorption alters facial structure. It creates a sunken look. More critically, it weakens support for nearby teeth.
Implants reverse this trend. The post acts like a root. It signals the bone to regenerate. Studies show implants preserve up to 90% of bone volume post-placement. This maintenance extends to facial contours. You avoid that aged appearance from tooth loss.
Jaw health links to broader stability. A robust bone base supports clear speech. It reduces headaches from misalignment. Patients notice sharper focus too. Stable bites ease TMJ discomfort. These gains compound into daily comfort.
In areas like Whitehouse, residents value long-term solutions. For those exploring dental implants in Whitehouse, TX, local expertise ensures tailored fits. This preserves bone while aligning with active lifestyles.
How Dental Implants Boost Nutritional Health
Chewing efficiency matters more than you think. Tooth loss limits food choices. Soft diets often skimp on fiber and proteins. This pattern risks deficiencies. Over years, it hampers immunity and muscle tone.
Implants restore bite force. They match natural teeth closely. Research indicates implant users consume 20% more varied nutrients. Crunchy veggies become feasible. Nuts and grains return to meals. Such diversity combats fatigue and supports heart health.
Oral health ties to digestion too. Thorough chewing breaks down food better. It eases gut workload. Fewer digestive woes mean steadier energy. Imagine vibrant days without mid-afternoon slumps.
The Oral-Systemic Connection: Beyond the Mouth
Your mouth serves as a health gateway. Bacteria from poor oral states can enter the bloodstream. This fuels inflammation elsewhere. Conditions like diabetes worsen with gum issues. Heart disease risks rise too.
Implants disrupt this cycle. They minimize plaque traps. Unlike dentures, they don’t rub gums raw. Cleanings stay routine. A 2023 study linked implant restoration to 15% lower systemic inflammation markers. Stable mouths foster calm bodies.
Mental perks shine here. Restored smiles build self-esteem. Social ease follows. Less anxiety over appearances frees mental space. This holistic lift enhances life quality profoundly.
Navigating Potential Challenges with Implants
No procedure lacks hurdles. Integration requires patience. Swelling or minor discomfort lingers briefly. Adhering to aftercare curbs most woes. Brushing and flossing around implants prevents peri-implantitis. This infection mimics gum disease but responds well to early vigilance.
Upper jaw placements demand care. Proximity to sinuses raises questions. Dental implants and sinus problems can arise if the bone is thin. Perforation risks temporary congestion or pain. Yet, advanced imaging spots issues pre-surgery. Bone grafts or sinus lifts resolve them safely. Most cases heal without lingering effects. Choose providers versed in these techniques for peace of mind.
Lifestyle factors play in. Smoking delays healing. Dry mouth from meds slows recovery. Addressing these upfront maximizes success.
Key Statistics on Implant Outcomes
To grasp implants’ reliability, consider these figures. They highlight why experts endorse them for health integration.
| Statistic |
Value |
Source Insight |
| Overall Success Rate |
95-98% |
Long-term studies (NIH) |
| 10-Year Survival Rate |
96.8% |
Clinical performance data |
| Bone Preservation Benefit |
Up to 90% maintained |
Jaw density research |
| Inflammation Reduction |
15% lower markers |
Systemic health links |
| Nutrient Intake Improvement |
20% more varied |
Dietary habit surveys |
These numbers underscore implants’ track record. They deliver enduring gains when paired with diligent care.
Actionable Tips for Implant Longevity
Ready to thrive with implants? Start with hygiene. Use soft brushes and antimicrobial rinses. Floss daily to shield the base. Schedule biannual checkups. Early spotting keeps complications at bay.
Diet tweaks help. Opt for balanced meals. Calcium-rich foods bolster bone. Avoid extremes like constant hard candies. They stress the crown.
Monitor changes. Sensitivity or looseness warrants a visit. Prompt action preserves health ties.
Stay hydrated. It combats dry mouth. This saliva boost fights bacteria naturally.
Trending FAQs on Dental Implants and Health
Curious about what others ask? Here’s a roundup of top Google queries. These address real concerns with straightforward answers.
- Are dental implants safe for overall health?
Yes, with a 95-98% success rate. They enhance bone health and reduce infection risks when placed by skilled pros.
- How do dental implants affect nutrition?
They restore chewing power, boosting nutrient absorption by up to 20%. This supports immunity and energy.
- Can implants improve cognitive function?
Emerging studies suggest yes. They may increase cerebral blood flow, aiding memory in older adults.
- What makes someone a good candidate?
Healthy gums, sufficient bone, and controlled chronic conditions. Consultations assess fit precisely.
- Do implants prevent facial changes?
Absolutely. They stimulate the jawbone, maintaining structure and youthful contours.
These insights demystify the process. Knowledge empowers confident steps.
If you are searching for a dentist in Whitehouse, TX, look for one who prioritizes comprehensive evaluations. They should discuss your health history openly. This builds trust from day one.
Embracing implants means investing in vitality. They weave oral care into whole-body wellness seamlessly.
As we wrap up, remember: a healthy mouth paves the way for a vibrant life. Implants aren’t just fixes. They’re bridges to better days. Feeling inspired? Reach out today. Call 903-328-6577 to schedule an appointment and unlock your health potential.







